Learning how to silence your inner critic after trauma can feel impossible. Personally, I developed a harsh (and loud) inner critic during early childhood following a trauma that made me question my worth. As I grew up, I found it "safer" to try to be the perfect kid, teen, young adult, and now woman, thinking maybe it would make me more worthy of love and good treatment. However, this has only ever perpetuated more self-loathing and vicious cycles.
PTSD Videos
Twenty years after being sexually assaulted, my childhood trauma made me sick. At the age of 24, I learned — the hard way — that if you ignore your emotions for too long, they will find other ways to get your attention, and even childhood trauma can make you sick.
Seeking validation from others is often demonized today. We are made to feel guilty for this human desire — for craving attention, reassurance, and support. And while it's healthy to give yourself the validation you're searching for, shaming yourself for seeking validation from others will not help you.
I’m Sammi Caramela, and I’m excited to join HealthyPlace as the new author of "Trauma! A PTSD Blog." I’ve lived most of my life in survival mode, but it wasn’t until I was in my early 20s that I realized I was suffering from posttraumatic stress disorder (PTSD) from early childhood trauma. Learning why I was suffering was crucial to healing from the extreme anxiety and depression I coped with on a regular basis.
Posttraumatic stress disorder (PTSD) and intimate relationships don't always go well together. On top of that, dating when you are in your 20s is tough. Finding people to date in real life is next to impossible, and online dating can be a fiasco. If you ask around, you'll find that many people in their 20s know and understand this struggle--myself being one of them. What most people don't understand, however, is how much more difficult dating and forming intimate relationships can be when you're suffering from PTSD.
Today I want to talk about why it's so difficult to follow through on New Year's resolutions when you have posttraumatic stress disorder (PTSD).
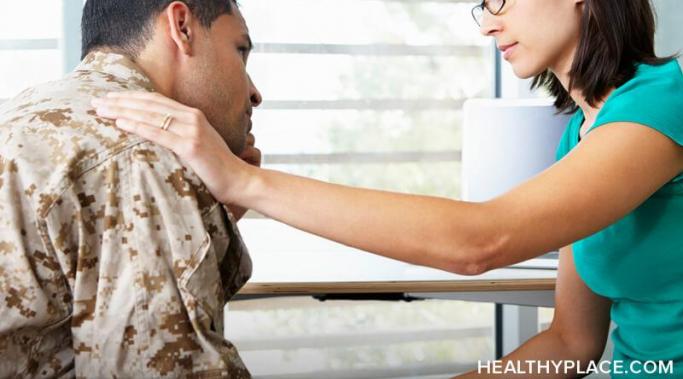
After going through a traumatic experience, it can be difficult to trust people and you can develop overwhelming trust issues. While many relationships are able to bounce back from difficult circumstances, around 5-10 percent of people with posttraumatic stress disorder (PTSD) will experience lasting relationship issues as a result of the traumatic experience.
My name is Bethany Avery, and I suffer from complex posttraumatic stress disorder (C-PTSD). I started showing symptoms of C-PTSD when I was 16 years old, and I first sought treatment for my disorder when I was in college. Finding solid footing in the shaky world that C-PTSD creates has been a tough but important battle, and I’m excited to share my story and coping methods as part of the "Trauma! A PTSD Blog" at HealthyPlace.
There are some false assumptions about posttraumatic stress disorder (PTSD) that people continue to make, and they make me want to hand out informational brochures on PTSD myths. Especially bothersome are the misconceptions rooted in PTSD stigma. Let's take a look at some of the more common examples of false assumptions about PTSD.
One of the things I find most frustrating about living with posttraumatic stress disorder (PTSD) is the impact PTSD has on my sex drive. I am a private person, and sex is a decidedly personal issue for many people, so I've put this topic off many times. However, the problems that PTSD can bring to partners don't go away on their own, so let's explore the potential difficulties that PTSD symptoms can bring to a sexual relationship.