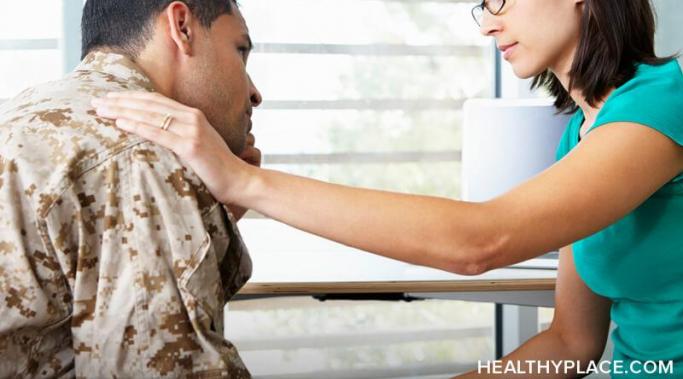
Developing intimate relationships when you have posttraumatic stress disorder (PTSD) can feel heavy, confusing, and downright terrifying at times. Growing up, I was a hypervigilant child, always trying to keep everyone safe. I didn't feel like I could trust anyone — especially not myself — and so I developed compulsions to forge a sense of control. I'd lock the door several times before bed, sometimes racing downstairs at 2 a.m. to check it was still locked. I'd turn down invites to sleepovers because I felt like I had to be with my parents in order to protect them (from what, I'm not sure). I'd ruminate for hours about the betrayals I'd faced and the roles I played in them. Posttraumatic stress disorder was making itself known in my relationships early.
About PTSD
Learning to trust yourself after trauma can feel like walking through a minefield. In my experience, if I take one wrong step, I fear my entire life will somehow implode. Even the most minor decisions send me into a fight-or-flight spiral. I deny my intuition and operate out of fear, craving a sense of security and certainty one simply cannot have in life. Learning to trust myself after trauma has been difficult.
Healing from my trauma required me to tell my trauma story — but not to over-identify with it. When I first began my healing journey, I would talk about my trauma to anyone who would listen: new friends, strangers on the Internet, distant family members, etc. In a way, telling my trauma story — and owning what I'd been through and how I got myself through it — empowered me. It gave me a sense of purpose and a feeling of pride; it also gifted me with much-needed validation.
I've found that emotional flashbacks are not as commonly discussed as "regular" flashbacks in posttraumatic stress disorder (PTSD). When I was first diagnosed with PTSD, I questioned my diagnosis because I hadn’t been experiencing the common symptom of a “flashback.” Flashbacks are a major part of PTSD, typically occurring in the form of visual memory and negatively stimulating our physical senses. However, I learned that many people — myself included — experience “emotional flashbacks,” or intense feelings of fear, shame, anger, and despair that are associated with a specific trauma.
Seeking validation from others is often demonized today. We are made to feel guilty for this human desire — for craving attention, reassurance, and support. And while it's healthy to give yourself the validation you're searching for, shaming yourself for seeking validation from others will not help you.
Suicide can be a tough topic to discuss among those suffering from posttraumatic stress disorder (PTSD). Though around 56% of people with PTSD experience suicidal thoughts, ideation, or actions, admitting to having those feelings can feel shameful. (Note: This post contains a trigger warning.)
Living with complex posttraumatic stress disorder (PTSD) is hard and it often makes life feel like a struggle. You may struggle to get out of bed, do your daily chores, put on a good face for those around you, or you may even feel like it's a struggle to live.
When you live with complex posttraumatic stress disorder (PTSD), flashbacks can be one of the most frustrating parts of it. You may go days, weeks, or months without one, then suddenly, bam, you’re hit with a new, frustrating flashback.
Black-and-white thinking is common to posttraumatic stress disorder (PTSD). When you are traumatized, especially repeatedly, you begin to believe that life is all good or all bad. Unfortunately, it’s more common to lean towards all bad, because that is what the traumatic experiences you lived through taught you.
Posttraumatic stress disorder (PTSD) stigma is alive and well. If you have PTSD, you've probably heard someone tell you to "just get over" your trauma. Maybe it was a well-meaning friend or family member, like my father who was frightened by my suicidal ideations. Or maybe it was a less well-meaning stranger, like the rude New Yorker who recently commented on my blog telling me to, "Grow up and take responsibility for [my] life." Whether the statement comes from a place of love or PTSD stigma, it doesn't make sense. Here's why.