Syndromes of Abnormal Sex Differentiation
I. Introduction
From the Johns Hopkins Children's Center, this booklet is designed to help parents and patients understand intersexuality and the challenges that accompany syndromes of "abnormal" sex differentiation.
Sexual differentiation is a complex process which results in a newborn baby who is either male or female. If errors in development occur, sexual development is abnormal and the sex organs of the baby are malformed. In such cases, individuals may develop both male and female characteristics. This is referred to as intersexuality.
Children born with deviations from normal development of the sex organs can be expected to grow up successfully and to lead enriched lives. However, their problems must be considered carefully. In cases of abnormal sex differentiation, efforts should be made to determine the reason for the abnormality as treatment may vary according to the cause of the disorder. There may also be a need for specific surgical repair and/or hormonal therapy. Finally, it is extremely important for parents and patients to have a good understanding of both the condition of sex differentiation that affects them, as well as possible ways for dealing with the condition. With this approach, patients will be better able to lead a fulfilled life, and to look forward to an education, career, marriage, and parenthood.
This booklet has been prepared to help parents and patients better understand intersexuality and the unique challenges that accompany syndromes of abnormal sex differentiation. We believe that informed individuals are better prepared to face these challenges and are more likely to meet successfully the demands of childhood, adolescence, and adulthood.
First, normal sex differentiation will be described. The understanding of this pattern of development will help patients and their families to understand the problems of ambiguous sex differentiation, which are subsequently outlined. Finally, a glossary of terms and a list of helpful support groups are provided.
II. Normal Sex Differentiation
Human sexual differentiation is a complicated process. In a simple manner, one can describe four major steps which constitute normal sexual differentiation. These four steps are:
- Fertilization and determination of genetic sex
- Formation of organs common to both sexes
- Gonadal differentiation
- Differentiation of the internal ducts and external genitalia
Step 1: Fertilization and Determination of Genetic Sex
The first step of sex differentiation takes place at fertilization. An egg from the mother, which contains 23 chromosomes (including an X chromosome), is combined with a sperm from the father, which also contains 23 chromosomes (including either an X or Y chromosome). Therefore, the fertilized egg has either a 46,XX (genetic female) or 46,XY (genetic male) karyotype.
Step 1 in sex differentiation: Determination of genetic sex
Egg (23,X) + Sperm (23,X)=46,XX genetic girl
OR
Egg (23,X) + Sperm (23, Y)=46, XY genetic boy
Step 2: Formation of Organs Common to Both Sexes
The fertilized egg multiplies to form a large number of cells, all of which are similar to each other. However, at specific times during the growth of an embryo, the cells differentiate to form the various organs of the body. Included in this development is the differentiation of the sex organs. At that stage, both 46,XX and 46,XY fetuses have similar sex organs, specifically:
- the gonadal ridges
- the internal ducts
- the external genitalia
a. The gonadal ridges can be easily recognized by 4-5 weeks of gestation. At that time, they already include the undifferentiated germ cells which will later develop into either eggs or sperm. The formation of gonadal ridges similar in both sexes is a prerequisite step to the development of differentiated gonads. This organization of cells into a ridge requires the effects of several genes, such as SF-1, DAX-1, SOX-9, etc. If any one of these genes is non-functional, then there is no formation of a gonadal ridge and therefore no formation of either testes or ovaries.
b. By 6-7 weeks of fetal life, fetuses of both sexes have two sets of internal ducts, the Mullerian (female) ducts and the Wolffian (male) ducts.
c. The external genitalia at 6-7 weeks gestation appear female and include a genital tubercle, the genital folds, urethral folds and a urogenital opening. (see Figure 2)
Step 3: Gonadal Differentiation
The important event in gonadal differentiation is the commitment of the gonadal ridge to become either an ovary or a testis.
a. In males, the gonadal ridge develops into testes as a result of a product from a gene located on the Y chromosome. This product has been termed the "testis determining factor" or "sex determining region of the Y chromosome" (SRY).
b. In females, the absence of SRY, due to the absence of a Y chromosome, permits the expression of other genes which will trigger the gonadal ridge to develop into ovaries.
Step 3 in Sex Differentiation: Determination of Gonadal Sex
XX fetus=ovary
(with no SRY)
OR
XY fetus=testes
(with SRY located on the Y chromosome)
Step 4: Differentiation of the Internal Ducts and External Genitalia
The next step in sex differentiation depends upon the formation of two important hormones: the secretion of Mullerian (female) Inhibiting Substance (MIS) and the secretion of androgens.
If testes are developing normally, then Sertoli cells of the developing testes produce MIS which inhibits the growth of the female Mullerian ducts (the uterus and fallopian tubes) which are present in all fetuses early in development. Additionally, the Leydig cells of the testes start secreting androgens. Androgens are hormones that produce growth effects on the male Wolffian ducts (the epididymis, vas deferens, seminal vesicles) which are also present in all fetuses early in development.
Unlike the testes, the ovaries do not produce androgens. As a result, the Wolffian ducts fail to grow and consequently disappear in fetuses with ovarian development. In addition, the ovaries do not produce MIS at the appropriate time, and as a consequence, the Mullerian (female) ducts can develop.
In other words, two products of the developing testes are needed for normal male development. First, MIS must be secreted to inhibit female duct growth and androgens must be secreted to enhance male duct growth. In contrast, a female fetus with no developing testes will produce neither MIS nor androgens, and hence female ducts will develop and male ducts will disappear.
Step 4 in Sex Differentiation: Determination of Internal Ducts
Males
Testes produce MIS=inhibit female development
Testes produce androgens=enhance male development
OR
Females
Ovaries do not produce MIS=enhance female development
Ovaries do not produce androgens=inhibit male development
External Genitalia
In the female, absence of androgens permits the external genitalia to remain feminine: the genital tubercle becomes the clitoris, the genital swellings become the labia majora and the genital folds become the labia minora.
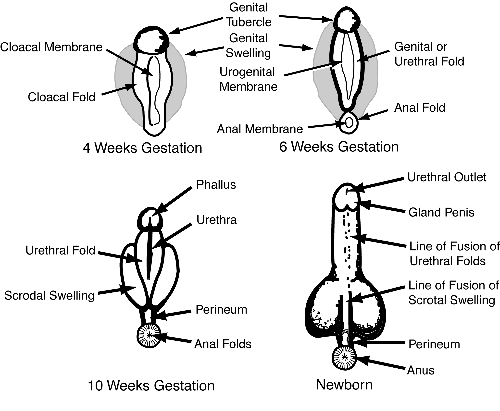
In the male, fetal androgens from the testes masculinize the external genitalia. The genital tubercle grows to become the penis and the genital swellings fuse to form the scrotum. The following diagrams illustrate each of these processes.
Figure 1
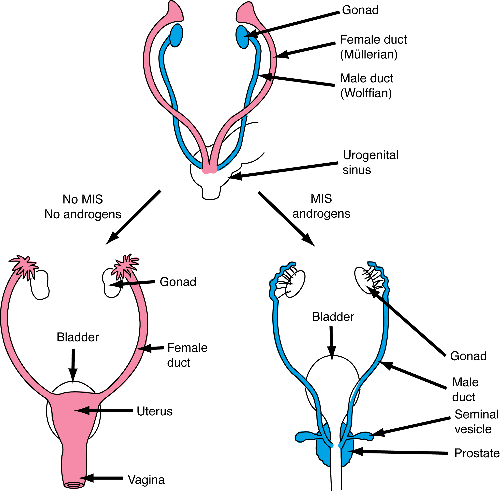
Figure 2
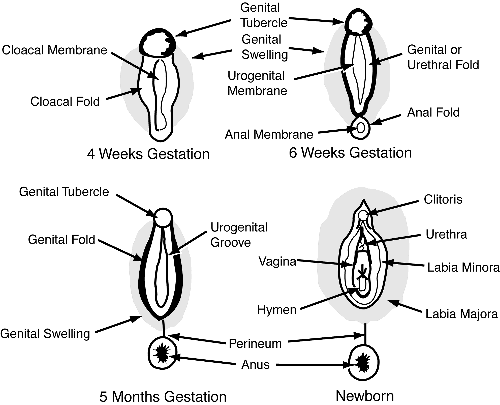
Figure 3
Summary of Normal Sex Differentiation
- genetic sex is determined
- testes develop in XY fetus, ovaries develop in XX fetus
- XY fetus produces MIS and androgens and XX fetus does not
- XY fetus develops Wolffian ducts and XX fetus develops Mullerian ducts
- XY fetus masculinizes the female genitalia to make it male and the XX fetus retains female genitalia
III. Disorders of Sex Differentiation - A General Outline
Sex differentiation is a complex physiological process comprised of many steps. Problems associated with sex differentiation, or syndromes of intersexuality, occur when errors in development take place at any
of these steps.
Genetic Sex
Problems can arise at fertilization when chromosomal sex is established. For example, girls with Turner Syndrome have a 45,XO karyotype and boys with Klinefelter Syndrome have a 47,XXY karyotype. It is also known that some women have a 46,XY or 47,XXX karyotype and some men a 46,XX or 47,XYY karyotype. Clearly then, when it is stated that 46,XY refers to male sex and 46,XX refers to female sex, this is a generalization which applies to most, but not all, individuals.
Gonadal Sex
Disorders of sex differentiation can occur when a bipotential gonad is incapable of developing into a testis or an ovary. The inability to develop testes may occur if a gene such as SRY is absent or deficient. When this is the case, a 46,XY fetus will not receive the SRY signal to develop testes despite the presence of a Y chromosome. Additionally, 46,XY fetuses may begin to develop testes, but this development can be thwarted, and subsequently MIS and androgen production may be absent or diminished.
Finally, the normal disappearance of germ cells associated with ovarian development in fetuses is so accelerated in Turner Syndrome that by birth these babies possess gonadal streaks as opposed to normal ovaries.
Mullerian and Wolffian Duct Development
Intersexuality can also result as a consequence of problems related to Mullerian or Wolffian duct development. For example, MIS secretion accompanied by the absence of androgens or the inability to respond to androgens can result in a fetus lacking both male and female internal duct structures. In contrast, the absence of MIS accompanied by androgen secretion can result in a fetus possessing both male and female internal duct structures to varying degrees.
External Genitalia
Babies born with sex differentiation syndromes possess external genitalia that can usually be classified as either:
- normal female
- ambiguous
- normal male but with a very small penis (micropenis)
Normal female external genitalia develop among 46,XY intersex patients when the genital tubercle, genital swellings, and genital folds either completely lack exposure to, or are totally incapable of responding to, male hormones. As a result, masculinization of the external genital structures is not possible. In such cases, the genital tubercle develops into a clitoris, the genital swellings develop into the labia majora and the genital folds develop into the labia minora.
Ambiguous external genitalia develop in female patients when the external genital structures are exposed to greater-than-normal amounts of male hormones (masculinized females) or in male patients when less-than-normal amounts of male hormones (under-masculinized males) occurs. Thus, in these patients, external genitalia develop in a manner that is neither female nor male, but rather is somewhere in between the two.
For instance, patients with ambiguous external genitalia may possess a phallus which ranges in size from resembling a large clitoris to a small penis. Additionally, these patients may possess a structure that resembles partially fused labia or a split scrotum. Finally, patients with ambiguous external genitalia often possess a urethral (urinary) opening that is not at the tip of the phallus (normal male position), but is instead located elsewhere on the phallus or perineum. The atypical positioning of the urethra in such instances is referred to as hypospadius.
Babies born with a penis that is much smaller than normal (micropenis) have a completely normal appearing external genitalia (i.e)., the urethra is properly located at the tip of the phallus and the scrotum is completely fused). However, the size of the phallus is closer to that of a normal clitoris than a normal penis.
IV. Specific Syndromes of Sex Differentiation
1. Androgen Insensitivity Syndrome (AIS)
Androgen Insensitivity Syndrome occurs when an individual, due to a mutation of the androgen receptor gene, is incapable of responding to androgens. Two forms of AIS exist, Complete AIS (CAIS) and Partial AIS (PAIS).
CAIS
CAIS affects 46,XY individuals. CAIS patients have normal appearing female external genitalia due to the their complete inability to respond to androgens. This is because the genital tubercle, genital swellings, and genital folds can not masculinize in these patients despite the presence of functional testes located in the abdomen. Similarly, Wolffian duct development does not occur because the Wolffian duct structures can not respond to androgens produced by CAIS patients. Mullerian duct development is inhibited in CAIS individuals because MIS is secreted by the testes.
In addition to possessing normal female external genitalia, CAIS individuals also experience normal female breast development along with sparse pubic and axillary hair growth at puberty. The following chart illustrates the steps of sex differentiation associated with CAIS compared to those of unaffected males and females.
| Normal Female Development | CAIS Development | Normal Male Development |
| XX | XY | XY |
| ovaries develop | testes develop | testes develop |
| no androgen produced | androgen produced, but body can not respond | androgen produced |
| Wolffian Ducts regress | Wolffian Ducts regress | Wolffian Ducts develop |
| no MIS produced | MIS produced | MIS produced |
| Mullerian Ducts develop | Mullerian Ducts do not develop | Mullerian Ducts do not develop |
| external genitalia are female | external genitalia are female | external genitalia are male |
| feminizing puberty | feminizing puberty without menses | masculinizing puberty |
PAIS
PAIS also affects 46,XY individuals. PAIS patients are born with ambiguous external genitalia due to their partial inability to respond to androgens. The genital tubercle is larger than a clitoris but smaller than a penis, a partially fused labia/scrotum may be present, the testes may be undescended, and perineal hypospadius is often present. Wolffian duct development is minimal or nonexistent and the Mullerian duct system does not develop properly.
PAIS patients will experience normal female breast development at puberty, along with a small amount of pubic and axillary hair. The chart on the following page illustrates the steps of sex differentiation associated with PAIS compared to those of unaffected males and females.
| Normal Female Development | PAIS Development | Normal Male Development |
| XX | XY | XY |
| ovaries develop | testes develop | testes develop |
| no androgen produced | androgen produced, but body partially unresponsive | androgen produced |
| Wolffian Ducts regress | Wolffian Ducts develop minimally | Wolffian Ducts develop |
| no MIS produced | MIS produced | MIS produced |
| Mullerian Ducts develop | Mullerian Ducts do not develop | Mullerian Ducts do not develop |
| external genitals are female | external genitalia are ambiguous | external genitalia are male |
| feminizing puberty | partial masculinizing puberty with testosterone therapy OR feminizing puberty with estrogen therapy | masculinizing puberty |
2. Gonadal Dysgenesis
Unlike AIS in which affected individuals possess functioning testes but can not respond to the androgens their testes produce, patients with Gonadal Dysgenesis can respond to androgens but develop abnormal testes which are incapable of producing androgens. Like AIS, two forms of Gonadal Dysgenesis exist (Complete and Partial).
Complete Gonadal Dysgenesis
Complete Gonadal Dysgenesis affects 46,XY individuals and is characterized by abnormally formed gonads which were originally on the path to testis differentiation (these abnormally formed gonads are referred to as gonadal streaks), female external genitalia, Mullerian duct development, and Wolffian duct regression. Female external genitalia develop due to the failure of the gonadal streaks to produce androgens necessary to masculinize the genital turbercle, genital swellings, and genital folds. Additionally, because the gonadal streaks are incapable of producing either androgens or MIS, the Wolffian duct system regresses while the Mullerian duct system develops. The following chart illustrates the steps of sex differentiation associated with Complete Gonadal Dysgenesis compared to those of unaffected males and females.
| Normal Female Development | Complete Gonadal Dysgenesis | Normal Male Development |
| XX | XY | XY |
| ovaries develop | streak gonads | testes develop |
| no androgen produced | no androgen produced | androgen produced |
| Wolffian Ducts regress | Wolffian Ducts regress | Wolffian Ducts develop |
| no MIS produced | no MIS produced | MIS produced |
| Mullerian Ducts develop | Mullerian Ducts develop | Mullerian Ducts regress |
| external genitalia are female | external genitalia are female | external genitalia are male |
| feminizing puberty | feminizing puberty with estrogen therapy | masculinizing puberty |
Partial Gonadal Dysgenesis
Partial Gonadal Dysgenesis also affects 46,XY individuals, and this condition is characterized by partial testes determination usually accompanied by ambiguous external genitalia at birth. Affected patients may have a combination of Wolffian and Mullerian duct development. The combination of both Wolffian and Mullerian duct development, along with ambiguity of the external structures, indicates that the testes produced more androgens and MIS than those of Complete Gonadal Dysgenesis patients, but not as much as would be seen in normal male development. The chart on the following page illustrates the steps of sex differentiation associated with Partial Gonadal Dysgenesis compared to those of unaffected males and females.
| Normal Female Development | Partial Gonadal Dysgenesis | Normal Male Development |
| XX | XY | XY |
| ovaries develop | partial testes determination | testes develop |
| no androgen produced | variable amount of androgen produced | androgen produced |
| Wolffian Ducts regress | some Wolffian Duct development | Wolffian Ducts develop |
| no MIS production | variable amount of MIS production | MIS production |
| Mullerian Ducts develop | some Mullerian Duct development | Mullerian Ducts do not develop |
| external genitalia are female | ambiguous external genitalia | external genitalia are male |
| feminizing puberty | feminizing puberty with estrogen therapy OR masculinizing puberty with testosterone therapy | masculinizing puberty |
3. 5![]() -Reductase Deficiency
-Reductase Deficiency
During fetal development, the genital tubercle, genital swellings, and genital folds masculinize when exposed to androgens. Androgens, or male hormones, are a general term for two specific hormones Ñ testosterone and dihydrotestosterone (DHT). DHT is a stronger androgen than testosterone, and DHT is formed when the enzyme 5![]() -Reductase converts testosterone to DHT.
-Reductase converts testosterone to DHT.
5-![]() reductase enzyme
reductase enzyme
Testosterone -----------a Dihydrotestosterone
5![]() -Reductase deficiency affects 46,XY individuals. During fetal development, the gonads differentiate into nomal testes, secrete appropriate amounts of testosterone, and patients are able to respond to this testosterone. However, affected individuals are unable to convert testosterone to DHT , and DHT is necessary for the external genitalia to masculinize normally. The result is a newborn baby with functioning testes, normally developed Wolffian ducts, no Mullerian ducts, a penis resembling a clitoris, and a
-Reductase deficiency affects 46,XY individuals. During fetal development, the gonads differentiate into nomal testes, secrete appropriate amounts of testosterone, and patients are able to respond to this testosterone. However, affected individuals are unable to convert testosterone to DHT , and DHT is necessary for the external genitalia to masculinize normally. The result is a newborn baby with functioning testes, normally developed Wolffian ducts, no Mullerian ducts, a penis resembling a clitoris, and a
scrotum resembling labia majora.
At puberty, testosterone (not DHT), is the essential androgen for masculinization of the external genitalia. Therefore, stereotypical signs of masculine pubertal development will be observed in patients. These signs include an increase in muscle mass, lowering of the voice, growth of the penis (although it is unlikely that it will reach a normal male length), and sperm production if the testes remain intact. These patients have a fair amount of pubic or axillary hair growth, but they have little or no facial hair. They do not experience female breast development. The following chart illustrates the steps of sex differentiation associated with 5![]() -Reductase Deficiency compared to those of unaffected males and females.
-Reductase Deficiency compared to those of unaffected males and females.
| Normal Female Development | 5 | Normal Male Development |
| XX | XY | XY |
| ovaries develop | testes develop | testes develop |
| no androgen produced | testosterone but no DHT produced | androgen produced |
| Wolffian Ducts regress | Wolffian Ducts develop | Wolffian Ducts develop |
| no MIS produced | MIS produced | MIS produced |
| Mullerian Ducts develop | Mullerian Ducts regress | Mullerian Ducts regress |
| external genitalia are female | ambiguous external genitalia | external genitalia are male |
| feminizing puberty | testes left intact, partial masculinizing puberty OR feminizing puberty with removal of testes and estrogen therapy | masculinizing puberty |
4. Testosterone Biosynthetic Defects
Testosterone is produced from cholesterol through a number of biochemical conversions. In some individuals, one of the enzymes needed for these conversions is deficient. In such cases, patients are unable to make normal amounts of testosterone despite the presence of testes. Testosterone Biosynthetic Defects affect 46,XY individuals and can be complete or partial, which leads to newborns who appear either completely female or ambiguous, respectively. Four Testosterone Biosynthetic Defects are
listed below:
- Cytochrome P450,CYP11A Deficiency
- 3B-Hydroxysteroid Dehydrogenase Deficiency
- Cytochrome P450,CYP17 Deficiency
- 17-Ketosteroid Reductase Deficiency
The first three enzyme deficiencies listed above result in Congenital Adrenal Hyperplasia (CAH) (described later) as well as decreased testosterone production by the testes. The fourth enzyme, 17-Ketosteroid Reductase Deficiency, is not associated with CAH. The following chart illustrates the steps of sex differentiation associated with Testosterone Biosynthetic Defects compared to those of unaffected males and females.
Complete Biosynthetic Defect
| Normal Female Development | Complete Testosterone Biosynthetic Defect | Normal Male Development |
| XX | XY | XY |
| ovaries develop | testes develop | testes develop |
| no androgen produced | no androgens due to enzyme deficiency | androgen produced |
| Wolffian Ducts regress | Wolffian Ducts regress | Wolffian Ducts develop |
| no MIS is produced | MIS is produced | MIS is produced |
| Mullerian Ducts develop | Mullerian Ducts regress | Mullerian Ducts regress |
| external genitalia are female | external genitalia are female | external genitalia are male |
| feminizing puberty | feminizing puberty if given estrogen therapy | masculinizing puberty |
Partial Biosynthetic Defect
| Normal Female Development | Partial Testosterone Biosynthetic Defect | Normal Male Development |
| XX | XY | XY |
| ovaries develop | testes develop | testes develop |
| no androgen produced | partial production of androgens | androgen produced |
| Wolffian Ducts regress | some Wolffian Duct development | Wolffian Ducts develop |
| no MIS produced | MIS produced | MIS produced |
| Mullerian Ducts develop | Mullerian Ducts regress | Mullerian Ducts regress |
| external genitalia are female | ambiguous external genitalia | external genitalia are male |
| feminizing puberty | partial masculinizing puberty with testosterone therapy OR feminizing puberty with estrogen therapy | masculinizing puberty |
5. Micropenis
Androgens are necessary at two different points in fetal development for a normal penis to form: (1) early in fetal life to masculinize the genital tubercle, genital swellings, and genital folds into a penis and scrotum, and (2) later in fetal life to enlarge the penis. Individuals with a micropenis possess a normally developed penis, except that the penis is extremely small. The condition of micropenis is thought to occur in 46,XY individuals if androgen production is insufficient for penile growth after the first part of masculinization of the external genitalia has already occurred. The chart on the following page illustrates the steps of sex differentiation associated with micropenis compared to those of unaffected males and females.
| Normal Female Development | Micropenis | Normal Male Development |
| XX | XY | |
| ovaries develop | testes develop | testes develop |
| no androgen produced | androgens early in fetal life, deficient later in fetal life | androgen produced |
| Wolffian Ducts regress | Wolffian Ducts develop | Wolffian Ducts develop |
| no MIS produced | MIS produced | MIS produced |
| Mullerian Ducts develop | Mullerian Ducts regress | Mullerian Ducts regress |
| external genitalia are female | micropenis | external genitalia are male |
| feminizing puberty | partially masculinizing puberty if exposed to testosterone OR feminizing puberty if given estrogen therapy | masculinizing puberty |
6. Timing Defect
The many steps of sex differentiation are further complicated by the fact that proper timing of these steps is necessary for normal development. If all of the steps required for male sex differentiation are working, yet these steps are delayed by even a few weeks, the result can be ambiguous differentiation of the external genitalia in a 46,XY individual. The following chart illustrates the steps of sex differentiation associated with a Timing Defect compared to those of normal males
| Normal Female Development | Timing Defect | Normal Male Development |
| XX | XY | XY |
| ovaries develop | testes develop | testes develop |
| no androgen produced | androgen produced at incorrect time | androgen produced |
| Wolffian Ducts regress | Wolffian Ducts develop | Wolffian Ducts develop |
| no MIS produced | MIS produced | MIS produced |
| Mullerian Ducts develop | Mullerian Ducts regress | Mullerian Ducts regress |
| external genitalia are female | external genitalia range from female to ambiguous | external genitalia are male |
| feminizing puberty | partially masculinizing puberty with testosterone therapy OR feminizing puberty with estrogen therapy | masculinizing puberty |
7. Congenital Adrenal Hyperplasia (CAH) in 46,XX Individals
In CAH excess adrenal androgens are produced as an indirect result of a cortisol biosynthetic defect (by far the most frequent defect is a cytochrome P450,CYP21 deficiency). In 46,XX individuals, excess adrenal androgens can lead to ambiguous development of the external genitalia, so that these babies have an enlarged clitoris and a fused labia which resembles a scrotum. The chart on the following page illustrates the steps of sexual differentiation associated with 46,XX CAH (21-hydroxylase deficiency) individuals compared to those of unaffected males and females.
| Normal Female Development | 46,XX CAH | Normal Male Development |
| XX | XX | XY |
| ovaries develop | ovaries develop | testes develop |
| no androgen produced | no testicular androgens but excessive adrenal androgens produced | androgen produced |
| Wolffian Ducts regress | Wolffian Ducts regress | Wolffian Ducts develop |
| no MIS produced | no MIS produced | |
| Mullerian Ducts develop | Mullerian Ducts develop | Mullerian Ducts regress |
| external genitalia are female | ambiguous external genitalia | external genitalia are male |
| feminizing puberty | feminizing puberty if treated with cortisol | masculinizing puberty |
8. Klinefelter Syndrome
Klinefelter Syndrome is the term given to individuals with a 47,XXY karyotype. At puberty Klinefelter men can experience female breast growth, low androgen production, small testes, and decreased sperm production. Additionally, although Klinefelter men undergo normal male differentiation of the external genitalia, they often possess a penis that is smaller than that of normal men. The following chart illustrates the steps of sexual differentiation associated with individuals who have Klinefelter Syndrome, compared to those of unaffected males and females.
| Normal Female Development | Klinefelter Syndrome | Normal Male Development |
| XX | XXY | XY |
| ovaries develop | small testes at puberty | testes develop |
| no androgen produced | often decreased androgen production | androgen produced |
| Wolffian Ducts regress | Wolffian Ducts develop | Wolffian Ducts develop |
| no MIS produced | MIS produced | MIS produced |
| Mullerian Ducts develop | Mullerian Ducts regress | Mullerian Ducts regress |
| external genitalia are female | male external genitalia with small penis | external genitalia are male |
| feminizing puberty | masculinizing puberty with possible decreased androgen production | masculinizing puberty |
9. Turner Syndrome
Turner Syndrome is the term given to individuals with a 45,XO karyotype. Turner patients can exhibit webbing of the neck, a broad chest, horseshoe kidneys, cardiovascular abnormalities, and short stature. Turner patients do not possess ovaries, but instead possess gonadal streaks. Turner patients have normal female external genitalia, but because they lack functioning ovaries (and thus the estrogens produced by ovaries) neither breast development, nor menstruation occurs spontaneously at puberty. The following chart illustrates the steps of sexual differentiation associated with Turner Syndrome compared to those of unaffected males and females.
| Normal Female Development | Turner Syndrome | Normal Male Development |
| XX | XO | XY |
| ovaries develop | gonadal streaks develop | testes develop |
| no androgen produced | no androgen produced | androgen produced |
| Wolffian Ducts regress | Wolffian Ducts regress | Wolffian Ducts develop |
| no MIS produced | no MIS produced | MIS produced |
| Mullerian Ducts develop | Mullerian Ducts develop | Mullerian Ducts regress |
| external genitalia are female | external genitalia are female | external genitalia are male |
| feminizing puberty | feminizing puberty with estrogen therapy | masculinizing puberty |
10. 45,XO/46,XY Mosaicism
Individuals born with 45,XO/46,XY Mosaicism can appear male, female, or ambiguous at birth. Males experience normal male sex differentiation and females are essentially identical to girls born with Turner Syndrome. For the purpose of this booklet, only patients with 45,XO/46,XY Mosaicism, who experience ambiguous sex differentiation, will be described on the following chart.
Mosaicism means that two or more sets of chromosomes influence the development of an individual. 45,XO/46,XY Mosaicism represents the most common mosaic condition involving the Y chromosome. Because the Y chromosome is affected, abnormal sex differentiation can result from this condition. The following chart illustrates the steps of sex differentiation associated with 45,XO/46,XY Mosaicism compared to those of unaffected males and females.
| Normal Female Development | 45,XO/46,XY Mosaicism | Normal Male Development |
| XX | XY | XY |
| ovaries develop | partial testes determination | testes develop |
| no androgen produced | variable amount of androgen produced | androgen produced |
| Wolffian Ducts regress | some Wolffian Duct development | Wolffian Ducts develop |
| no MIS production | MIS production | |
| Mullerian Ducts develop | some Mullerian Duct development | Mullerian Ducts do not develop |
| external genitalia are female | ambiguous external genitalia | external genitalia are male |
| feminizing puberty | feminizing puberty with estrogen therapy OR masculinizing puberty with testosterone therapy | masculinizing puberty |
V. Summary
Sexual differentiation refers to the physiological development of a fetus along male or female lines. Disorders of sexual differentiation, or syndromes of intersexuality, result when errors occur at any of these steps. This booklet is organized to serve as a basic explanation of the process of normal sexual differentiation, and it is also meant to explain the deviations from normal development underlying several syndromes of sexual differentiation.
Endocrine Treatment
1. What is the procedure for identifying and treating intersex syndromes in newborns?
When a child with an intersex syndrome also has ambiguous (undifferentiated) external genitalia, the syndrome is usually identified at birth. We recommend that a team consisting of a pediatric endocrinologist, gynecologist, urologist, geneticist and psychologist experienced in dealing with intersex conditions work together to treat these children.
Although difficult for parents, it is important not to assign a sex to an affected newborn until after proper diagnosis is agreed upon by the parents and team of doctors. We think this because it is more difficult for families to reassign a baby's sex than to postpone an initial assignment until after a diagnosis is agreed upon.
The examinations and laboratory tests necessary for attempting to establish a diagnosis may take several days. During that time, we advise parents to report to well-wishers that the infant was born with incompletely developed genitalia, and that it may take several days before the sex of the baby can be determined.
Until a diagnosis is made, it is important to use neutral terms such as baby, gonad and phallus instead of sex-specific terms like boy or girl, testes or ovaries and penis or clitoris. By using neutral terms, it is easier for families to adopt the appropriate sex of assignment for the child after a diagnosis has been made.
The following chart shows the recommended schedule for diagnostic tests and examinations for establishing a diagnosis as quickly and as accurately as possible.
Each day, weigh infant and check levels of serum electrolytes and blood glucose
- Day 1: karyotype
- Day 2: plasma testosterone, dihydrotestosterone,androstenedione
- Day 3: plasma 17-hydroxyprogesterone, 17-hydroxypregnenolone, androstenedione
- Day 4: sonogram for gonads and uterus, genitogram with or without IVP
- Day 5:repeat plasma 17-hydroxyprogesterone, 17 hydroxypregnenolone, androstenedione
The karyotype determines if a child is 46,XX, 46,XY, or a variant of the two. Androgens should be measured on Day 2 because the concentrations of these hormones decrease after that time. 17-hydroxyprogesterone, progesterone and androstenedione may be elevated after birth, but by Day 3 it is possible to detect abnormal concentrations of these hormones. Both a sonogram and genitogram allow physicians to determine which parts of the Mullerian and Wolffian duct system are present, and where they are located. In some cases, a stimulation test with human chorionic gonadotropin (HCG) is used to determine the nature of steroid secretion of the gonads, particularly if the exam is after 3 months of age. Studies on Day 5 will confirm values obtained on previous days. Finally, it is extremely important to closely monitor weight, serum electrolytes and blood glucose levels to assure that the newborn will not experience an adrenal crisis, a common occurrence in some syndromes of sex differentiation.
2. What is the procedure for identifying and treating intersex syndromes in older children?
While we recommend that sex assignment be postponed until after a diagnosis is made for a newborn with an intersex syndrome, older infants or children will have already lived as either a boy or girl regardless of diagnosis. In such instances, it is usually best to continue with the original sex assignment because such a change is often unsuccessful if it occurs after the first 18 months of life. We feel that sex reassignment within the first month of life is most likely to be successful if such a change is determined necessary by parents and doctors. For most older children, a reassignment should only be considered if desired by the child.
After 3 months of age and before puberty, one often uses an HCG test to determine if the gonad can secrete androgens. This is accomplished by administering a series of injections of human chorionic gonadotropin (HCG).
3. What are the goals of endocrine treatment for intersex patients ?
For patients raised as males, the goals of endocrine treatment are to encourage masculine development, and correspondingly suppress feminine development, of sexual characteristics. For example, increased penile size, hair distribution and body mass can be accomplished for some individuals through the use of testosterone treatment.
For patients raised as females, the goals of treatment are to simultaneously encourage feminine development and discourage masculine development of sexual characteristics. For example, breast development and menstruation can occur for some individuals following estrogen treatment.
In addition to sex hormones, patients with Congenital Adrenal Hyperplasia may also take glucocorticoids and salt-retaining hormones. Glucocorticoids can help these patients maintain appropriate reactions to physical stress as well as suppress unwanted masculine sexual development in female patients.
4. How long do patients need to take their hormone treatments?
Sex hormone therapy is usually initiated at puberty and glucocorticoids are administered when appropriate much earlier, usually at the time of diagnosis. Whether patients take male hormones, female hormones or glucocorticoids, it is important to continue with these medications throughout life. For example, male hormones are needed in adulthood to maintain masculine sexual characteristics, female hormones to protect against osteoporosis and cardiovascular disease, and glucocorticoids to protect against hypoglycemia and stress-related illnesses.
Surgical Treatment
1. What is the goal of reconstructive female genital surgery?
The goal of reconstructive female genital surgery is to have external feminine genitalia which look as normal as possible and will be correct for sexual function. The first step is to reduce the size of the markedly enlarged clitoris while preserving the nerve supply to the clitoris, and to place it in the normal female hidden position. The second step is to exteriorize the vagina so that it comes to the outside of the body in the area just below the clitoris.
The first step is usually more appropriate early in life. The second step is probably more successful when the patient is ready to start her sex life.
2. What are the goals of reconstructive male genital surgery?
The major goals are to straighten the penis, and to move the urethra from wherever it lies to the tip of the penis. This can be done in one step. However, in many cases, it will take more than one step particularly if the amount of available skin is limited, the curvature of the penis is marked, and the overall condition is severe.
3. What are the pros and cons of early surgery vs. late surgery in the male sex of rearing?
As far as male sex of rearing is concerned, early surgery can be performed easily between the ages of 6 months and 11/2 years. Generally speaking, it is better to try to obtain full correction of the genitalia before the child is two years of age, when he will be less aware of the problems related to surgery.
Late surgery in males would be defined after two years of age. Most male surgery should be performed early in life and should not be postponed until adolescence.
4. What are the pros and cons of early surgery vs. late surgery in the female sex of rearing?
As far as female sex of rearing is concerned, when the vaginal opening is easily reached and the clitoris is not markedly enlarged, exteriorization of the vagina without clitoral correction can be done early in life. If there is a great deal of masculinization with a markedly enlarged clitoris and an almost closed vagina (or a vagina located high and very posterior), then it is often advised to postpone exteriorization of the vagina until adolescence.
There are two distinct schools of thought in reconstructive surgery today concerning bringing the vagina down to the normal female position. Some people recommend that this all be done in infancy so that the entire reconstruction is complete by two years of age, accepting that mild complications may occur later in life. Others think that the surgery should be postponed until puberty, until the girl is under the influence of estrogen and the vagina can be brought down more easily when the young woman is ready to begin her sex life.
5. What are the complications associated with each type of procedure?
In male reconstructive surgery the complications include failure to get the penis straight, resulting in continued bending of the penis. Another complication would be a fistula or leak in the reconstructed male urethra. Neither one of these are severe complications presently and can be repaired without a great deal of difficulty. However, successful reconstruction does not result in a fully normal penis, as a rebuilt urethra is not surrounded by normal spongious tissue (corpus), nor does surgery correct the size of the penis.
In female reconstructive surgery, complications depend on the location of the vagina. One complication that can occur is that scar tissue forms where the vagina exits the inside of the body and causes stenosis or narrowing of the entrance to the vagina. With a high vagina, which is up near the bladder neck in the urinary control area (sphincter), the urinary control mechanism could be damaged and the child could become incontinent of urine as a result. This is why surgery should be performed by a surgeon who is experienced in dealing with birth defects of this magnitude. On occasion, it is necessary to reconstruct a neo-vagina. In such cases, the neo-vagina is normally functional but it may not look like normal female genitalia.
6. On average, how many surgeries are needed to obtain a desirable cosmetic and functional result?
In males, this depends on the location of the urethra, the amount of available skin and the degree of bending of the penis. In favorable cases, the maximum number of operations can be two or three.
In females with a low vagina and a slightly enlarged clitoris, usually one operation is performed in infancy, followed often by a "touch up" operation in adolescence. In females with a high vagina, surgery in infancy feminizes the external genitalia, with subsequent surgery to bring down the vagina in late childhood or
early adolescence, depending on the preference of the patient.
7. What is required for post-surgical maintenance in females?
We usually do not advise vaginal dilation in our young patients because we think this is stressful, both on parents and children. However, dilation may be needed in post-pubertal women. We do accept the fact that some patients may need touch up surgery when they are older.
Psychological Treatment For Intersex Patients
1. Who should receive counseling?
In our opinion, all intersex patients and family members should seriously consider counseling. Counseling can be provided by a pediatric endocrinologist, psychologist, psychiatrist, clergyman, genetic counselor or other individual the family is comfortable talking with. It is important, however, that the individual offering counseling services be very familiar with diagnostic and treatment issues related to intersex conditions. Additionally, it is helpful if the counselor has a background in sex therapy or sex counseling.
The following topics are often addressed during counseling sessions: knowledge about condition and treatment, infertility, sexual orientation, sexual function and genetic counseling. At different times throughout their lives, we think that all patients and parents are troubled by a number of these topics and could therefore benefit from counseling.
2. How long do patients and family members need to see a counselor?
Each person is different in their need for counseling. We believe individuals benefit from talking to a counselor throughout life, but that the need to do so may increase or decrease at different points in development. For example, parents may seek the service of a counselor more frequently as their child ages and subsequently asks more questions about their condition. Additionally, patients may find it particularly helpful to seek the services of a counselor once they have decided to become sexually active.
Glossary of Terms
- Adrenal glands:
- a pair of glands in males and females, located above the kidneys, which produce a number of hormones, including androgens
- Androgens:
- the main hormones testosterone and dihydrotestosterone secreted from the testes
- Estrogen:
- the primary hormones produced by the ovaries
- Genital folds:
- common to both males and females early in development. In males the genital folds develop into the scrotum and in females develop into the labia majora
- Genital ridges:
- fetal tissue that can develop into either an ovary or a testis
- Genital tubercle:
- common to both males and females early in development. In males the genital tubercle develops into a penis and in females develops into the clitoris.
- Intersexuality:
- An alternative term for hermaphroditism
- Karyotype:
- A photograph of a person's chromosomes, arranged according to size
- Mullerian ducts:
- A system present in both sexes early in fetal development. Upon development this system differentiates into a uterus, fallopian tubes and posterior portion of the vagina.
- Mullerian Inhibiting Substance (MIS):
- Produced by the Sertoli cells, and inhibits Mullerian duct formation
- Ovary:
- female gonad which manufactures estrogens and eggs
- SRY:
- a gene on the Y chromosome whose product instructs the fetal germinal ridge to develop into a testis
- Testes:
- male gonad which manufactures testosterone and sperm
- Urethral folds:
- common to both males and females early in development, in males the urethral folds develop into the urethra and corpora and in females into the labia minora.
- Wolffian ducts:
- a system present in both sexes early in fetal development; upon development, this system differentiates into the epididymis, vas deferens, and seminal vesicles
Intersex Support Group Contact Information
Some of the Available Support Groups for Individuals Affected by Syndromes of Abnormal Sexual Differentiation
- Androgen Insensitivity Syndrome Support Group (AISSG)
http://www.medhelp.org/www/ais - Intersex Society of North America
http://www.isna.org/ - Klinefelter Syndrome and Associates
http://www.genetic.org/ - Magic Foundation for Children's Growth
http://www.magicfoundation.org/www - The Turner Syndrome Society of the United States
http://www.turnersyndrome.org/
next: A Single Word: Stop!
~ all inside intersexuality articles
~ all articles on gender
APA Reference
Staff, H.
(2007, August 9). Syndromes of Abnormal Sex Differentiation, HealthyPlace. Retrieved
on 2026, April 2 from https://www.healthyplace.com/gender/inside-intersexuality/syndromes-of-abnormal-sex-differentiation

