About a month ago, I talked about getting my child evaluated for attention-deficit/hyperactivity disorder (ADHD). Technically, though, it wasn't a formal evaluation. It was basically a request (or plea, however you want to look at it) for my child's insurance company to foot the bill for ADHD testing. It was supposed to be the first step in getting the help we needed. Unfortunately, the insurance company decided it would also be the last step. They denied our request, even though the doctor thought ADHD testing was warranted. We're right back where we started.
Mental Health Treatment - Parenting Child with Mental Iillness
When choosing a topic to write about for "Life with Bob," I usually like to try to pick just the right one, maybe even do some research to see what my readers are asking about on Google. This week, though, I can only think about one thing: my child with attention-deficit/hyperactivity disorder (ADHD) won't listen to me.
My child is going through a formal evaluation for his attention-deficit/hyperactivity disorder (ADHD), which means I've answered approximately 506 questions regarding everything from how he acts in school to how I discipline him at home to which daily tasks he can accomplish by himself without being prompted. The doctor also took notes on how I interacted with my son, and by the end of the session, I felt like I had been evaluated as a mother as much as my child had been evaluated for ADHD. I felt insecure and judged.
A little while ago, I wrote a post about how I'm okay with my child having a mental illness. More recently, I was thrilled to learn that he feels the same way. My child wants to keep his attention-deficit/hyperactivity disorder (ADHD), and he isn't a fan of the idea of someone taking it away.
Can you teach self-regulation to children with disruptive mood dysregulation disorder (DMDD) when the inability to self-regulate emotions is the hallmark of the disorder? Anything and everything seems to trigger emotional meltdowns. What can we do as parents and caregivers, especially when we feel so frazzled ourselves? A few strategies for teaching self-regulation for children with DMDD do exist.
The transition from your teen's inpatient psychiatric care facility to home can mark an exciting change for your child. However, without a detailed plan for her transition, leaving inpatient psychiatric care can exacerbate her mental illness issues. Creating a solid plan for the transition period after your teen's inpatient psychiatric care can help your child be a success as she transitions back into regular life (Coping with Life After Residential Mental Health Treatment).
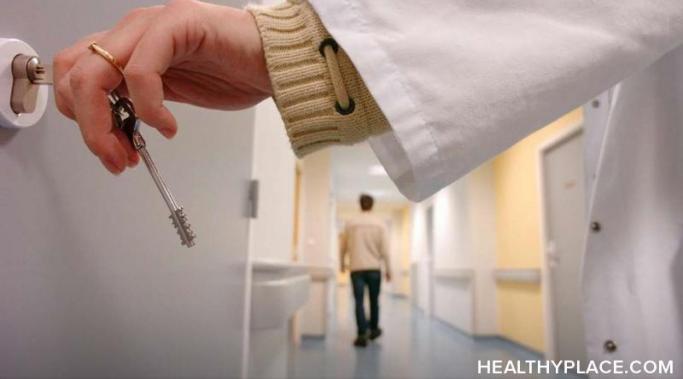
Putting a child in residential psychiatric care is one of the hardest decisions a parent has to make. Five years ago, I put my teenager into a residential psychiatric care facility for a year. Housing my child out of my home and in a residential mental health treatment center was a very painful decision that probably saved—and definitely changed—my child’s life.
The main symptom of disruptive mood dysregulation disorder (DMDD) is chronic irritability. "Irritability" is a vague word, though. It doesn't adequately describe how angry and mean our kids with DMDD can get or how demoralizing it feels. As parents, we work hard to raise decent human beings, then a DMDD outburst erupts and that decency seemingly flies out the door.
February is Teen Dating Violence Awareness Month (TDVAM), spotlighting the fact that every year "approximately 1.5 million high school students nationwide experience physical abuse from a dating partner," according to the Domestic Violence Awareness Project. Awareness of violence in teen and 20-something dating is an important key to turning these statistics around, especially in teens with mental illness, yet three out of four parents never talk to their children about domestic violence. As parents of mentally ill children, it is vital that we address this issue and speak to our teens about dating violence and what to do.
At 18, when our mentally ill children are no longer minors, it is important to encourage them to waive their privacy rights through the Health Insurance Portability and Accountability Act (HIPAA) and allow parents to participate on their mental health team. To assure that adult children waive their privacy rights, parents need to develop a relationship of trust.