Diabetes Sex and Urological Problems

Diabetes can cause sexual and urological problems in both men and women. Discover the causes and treatments for these diabetes complications.
Contents:
- Diabetes and Sexual Problems
- What sexual problems can occur in men with diabetes?
- What sexual problems can occur in women with diabetes?
- Diabetes and Urologic Problems
- Who is at risk for developing sexual and urologic problems of diabetes?
- Can diabetes-related sexual and urologic problems be prevented?
- Points to Remember
Troublesome bladder symptoms and changes in sexual function are common health problems as people age. Having diabetes can mean early onset and increased severity of these problems. Sexual and urologic complications of diabetes occur because of the damage diabetes can cause to blood vessels and nerves. Men may have difficulty with erections or ejaculation. Women may have problems with sexual response and vaginal lubrication. Urinary tract infections and bladder problems occur more often in people with diabetes. People who keep their diabetes under control can lower their risk of the early onset of these sexual and urologic problems.
+++
Diabetes and Sexual Problems
Both men and women with diabetes can develop sexual problems because of damage to nerves and small blood vessels. When a person wants to lift an arm or take a step, the brain sends nerve signals to the appropriate muscles. Nerve signals also control internal organs like the heart and bladder, but people do not have the same kind of conscious control over them as they do over their arms and legs. The nerves that control internal organs are called autonomic nerves, which signal the body to digest food and circulate blood without a person having to think about it. The body's response to sexual stimuli is also involuntary, governed by autonomic nerve signals that increase blood flow to the genitals and cause smooth muscle tissue to relax. Damage to these autonomic nerves can hinder normal function. Reduced blood flow resulting from damage to blood vessels can also contribute to sexual dysfunction.
What sexual problems can occur in men with diabetes?
Erectile Dysfunction
Erectile dysfunction is a consistent inability to have an erection firm enough for sexual intercourse. The condition includes the total inability to have an erection and the inability to sustain an erection.
Estimates of the prevalence of erectile dysfunction in men with diabetes vary widely, ranging from 20 to 75 percent. Men who have diabetes are two to three times more likely to have erectile dysfunction than men who do not have diabetes. Among men with erectile dysfunction, those with diabetes may experience the problem as much as 10 to 15 years earlier than men without diabetes. Research suggests that erectile dysfunction may be an early marker of diabetes, particularly in men ages 45 and younger.
In addition to diabetes, other major causes of erectile dysfunction include high blood pressure, kidney disease, alcohol abuse, and blood vessel disease. Erectile dysfunction may also occur because of the side effects of medications, psychological factors, smoking, and hormonal deficiencies.
Men who experience erectile dysfunction should consider talking with a health care provider. The health care provider may ask about the patient's medical history, the type and frequency of sexual problems, medications, smoking and drinking habits, and other health conditions. A physical exam and laboratory tests may help pinpoint causes of sexual problems. The health care provider will check blood glucose control and hormone levels and may ask the patient to do a test at home that checks for erections that occur during sleep. The health care provider may also ask whether the patient is depressed or has recently experienced upsetting changes in his life.
Treatments for erectile dysfunction caused by nerve damage, also called neuropathy, vary widely and range from oral pills, a vacuum pump, pellets placed in the urethra, and shots directly into the penis, to surgery. All of these methods have advantages and disadvantages. Psychological counseling to reduce anxiety or address other issues may be necessary. Surgery to implant a device to aid in erection or to repair arteries is usually used as a treatment after all others fail.
Retrograde Ejaculation
Retrograde ejaculation is a condition in which part or all of a man's semen goes into the bladder instead of out the tip of the penis during ejaculation. Retrograde ejaculation occurs when internal muscles, called sphincters, do not function normally. A sphincter automatically opens or closes a passage in the body. With retrograde ejaculation, semen enters the bladder, mixes with urine, and leaves the body during urination without harming the bladder. A man experiencing retrograde ejaculation may notice that little semen is discharged during ejaculation or may become aware of the condition if fertility problems arise. Analysis of a urine sample after ejaculation will reveal the presence of semen.
Poor blood glucose control and the resulting nerve damage can cause retrograde ejaculation. Other causes include prostate surgery and some medications.
For additional information about erectile dysfunction, see the fact sheet Erectile Dysfunction, available from the National Kidney and Urologic Diseases Information Clearinghouse at 1-800-891-5390.
Retrograde ejaculation caused by diabetes or surgery may be helped with a medication that strengthens the muscle tone of the sphincter in the bladder. A urologist experienced in infertility treatments may assist with techniques to promote fertility, such as collecting sperm from the urine and then using the sperm for artificial insemination.
What sexual problems can occur in women with diabetes?
Many women with diabetes experience sexual problems. Although research about sexual problems in women with diabetes is limited, one study found 27 percent of women with type 1 diabetes experienced sexual dysfunction. Another study found 18 percent of women with type 1 diabetes and 42 percent of women with type 2 diabetes experienced sexual dysfunction.
Sexual problems may include
- decreased vaginal lubrication, resulting in vaginal dryness
- uncomfortable or painful sexual intercourse
- decreased or no desire for sexual activity
- decreased or absent sexual response
Decreased or absent sexual response can include the inability to become or remain aroused, reduced or no sensation in the genital area, and the constant or occasional inability to reach orgasm.
Causes of sexual problems in women with diabetes include nerve damage, reduced blood flow to genital and vaginal tissues, and hormonal changes. Other possible causes include some medications, alcohol abuse, smoking, psychological problems such as anxiety or depression, gynecologic infections, other diseases, and conditions relating to pregnancy or menopause.
Women who experience sexual problems or notice a change in sexual response should consider talking with a health care provider. The health care provider will ask about the patient's medical history, any gynecologic conditions or infections, the type and frequency of sexual problems, medications, smoking and drinking habits, and other health conditions. The health care provider may ask whether the patient might be pregnant or has reached menopause and whether she is depressed or has recently experienced upsetting changes in her life. A physical exam and laboratory tests may also help pinpoint causes of sexual problems. The health care provider will also talk with the patient about blood glucose control.
Prescription or over-the-counter vaginal lubricants may be useful for women experiencing vaginal dryness. Techniques to treat decreased sexual response include changes in position and stimulation during sexual relations. Psychological counseling may be helpful. Kegel exercises that help strengthen the pelvic muscles may improve sexual response. Studies of drug treatments are under way.
Diabetes and Urologic Problems
Urologic problems that affect men and women with diabetes include bladder problems and urinary tract infections.
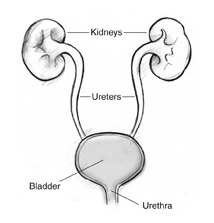
The urinary tract.
Bladder Problems
Many events or conditions can damage nerves that control bladder function, including diabetes and other diseases, injuries, and infections. More than half of men and women with diabetes have bladder dysfunction because of damage to nerves that control bladder function. Bladder dysfunction can have a profound effect on a person's quality of life. Common bladder problems in men and women with diabetes include the following:
- Overactive bladder. Damaged nerves may send signals to the bladder at the wrong time, causing its muscles to squeeze without warning. The symptoms of overactive bladder include
- urinary frequency—urination eight or more times a day or two or more times a night
- urinary urgency—the sudden, strong need to urinate immediately
- urge incontinence—leakage of urine that follows a sudden, strong urge to urinate
- Poor control of sphincter muscles. Sphincter muscles surround the urethra—the tube that carries urine from the bladder to the outside of the body—and keep it closed to hold urine in the bladder. If the nerves to the sphincter muscles are damaged, the muscles may become loose and allow leakage or stay tight when a person is trying to release urine.
- Urine retention. For some people, nerve damage keeps their bladder muscles from getting the message that it is time to urinate or makes the muscles too weak to completely empty the bladder. If the bladder becomes too full, urine may back up and the increasing pressure may damage the kidneys. If urine remains in the body too long, an infection can develop in the kidneys or bladder. Urine retention may also lead to overflow incontinence—leakage of urine when the bladder is full and does not empty properly.
Diagnosis of bladder problems may involve checking both bladder function and the appearance of the bladder's interior. Tests may include x rays, urodynamic testing to evaluate bladder function, and cystoscopy, a test that uses a device called a cystoscope to view the inside of the bladder.
Treatment of bladder problems due to nerve damage depends on the specific problem. If the main problem is urine retention, treatment may involve medication to promote better bladder emptying and a practice called timed voiding—urinating on a schedule—to promote more efficient urination. Sometimes people need to periodically insert a thin tube called a catheter through the urethra into the bladder to drain the urine. Learning how to tell when the bladder is full and how to massage the lower abdomen to fully empty the bladder can help as well. If urinary leakage is the main problem, medications, strengthening muscles with Kegel exercises, or surgery can help. Treatment for the urinary urgency and frequency of overactive bladder may involve medications, timed voiding, Kegel exercises, and surgery in some cases.
Urinary Tract Infections
Infections can occur when bacteria, usually from the digestive system, reach the urinary tract. If bacteria are growing in the urethra, the infection is called urethritis. The bacteria may travel up the urinary tract and cause a bladder infection, called cystitis. An untreated infection may go farther into the body and cause pyelonephritis, a kidney infection. Some people have chronic or recurrent urinary tract infections. Symptoms of urinary tract infections can include
- a frequent urge to urinate
- pain or burning in the bladder or urethra during urination
- cloudy or reddish urine
- in women, pressure above the pubic bone
- in men, a feeling of fullness in the rectum
If the infection is in the kidneys, a person may have nausea, feel pain in the back or side, and have a fever. Frequent urination can be a sign of high blood glucose, so results from recent blood glucose monitoring should be evaluated.
The health care provider will ask for a urine sample, which will be analyzed for bacteria and pus. Additional tests may be done if the patient has frequent urinary tract infections. An ultrasound exam provides images from the echo patterns of sound waves bounced back from internal organs. An intravenous pyelogram uses a special dye to enhance x-ray images of the urinary tract. Cystoscopy might be performed.
Early diagnosis and treatment are important to prevent more serious infections. To clear up a urinary tract infection, the health care provider will probably prescribe antibiotic treatment based on the type of bacteria in the urine. Kidney infections are more serious and may require several weeks of antibiotic treatment. Drinking plenty of fluids will help prevent another infection.
The National Kidney and Urologic Diseases Information Clearinghouse, at www.kidney.niddk.nih.gov or 1-800-891-5390, offers additional information about urologic problems.
Who is at risk of developing sexual and urologic problems of diabetes?
Risk factors are conditions that increase the chances of getting a particular disease. The more risk factors people have, the greater their chances of developing that disease or condition. Diabetic neuropathy and related sexual and urologic problems appear to be more common in people who
- have poor blood glucose control
- have high levels of blood cholesterol
- have high blood pressure
- are overweight
- are older than 40
- smoke
- are physically inactive
Can diabetes-related sexual and urologic problems be prevented?
People with diabetes can lower their risk of sexual and urologic problems by keeping their blood glucose, blood pressure, and cholesterol levels close to the target numbers their health care provider recommends. Being physically active and maintaining a healthy weight can also help prevent the long-term complications of diabetes. For those who smoke, quitting will lower the risk of developing sexual and urologic problems due to nerve damage and also lower the risk for other health problems related to diabetes, including heart attack, stroke, and kidney disease.
Points to Remember
The nerve damage of diabetes may cause sexual or urologic problems.
- Sexual problems in men with diabetes include
- erectile dysfunction
- retrograde ejaculation
- Sexual problems in women with diabetes include
- decreased vaginal lubrication and uncomfortable or painful intercourse
- decreased or no sexual desire
- decreased or absent sexual response
- Urologic problems in men and women with diabetes include
- bladder problems related to nerve damage, such as overactive bladder, poor control of sphincter muscles, and urine retention
- urinary tract infections
- Controlling diabetes through diet, physical activity, and medications as needed can help prevent sexual and urologic problems.
- Treatment is available for sexual and urologic problems.
Source: NIH Publication No. 09-5135, December 2008
APA Reference
Staff, H.
(2022, January 4). Diabetes Sex and Urological Problems, HealthyPlace. Retrieved
on 2026, March 29 from https://www.healthyplace.com/diabetes/complications/diabetes-sex-and-urological-problems



