Supporting an ADHD Child in the Classroom
Detailed information on ADHD children in the classroom: How ADHD affects a child's learning ability, ADHD medication during school, and helpful school accommodations for children with ADHD.
What is ADHD?
Attention Deficit Hyperactivity Disorder is a neuro-developmental disorder, the symptoms of which evolve over time. It is considered to have three core factors, involving inattention, hyperactivity and impulsivity. In order to have a diagnosis of ADHD the child would need to show significant problems relating to these three factors which would then constitute an impairment in at least two different settings, usually home and school.
The child with ADHD is easily distracted, forgets instruction and tends to flit from task to task. At other times they may by fully focused on an activity, usually of their choice. Such a child may also be over-active, always on the go physically. They are often out of their seat and even when seated are restless, fidgety or shuffling. The phrase "rump hyperactivity" has been coined to describe this wriggling restlessness often seen in children with ADHD when they are required to sit in one place for a length of time. Often children with ADHD will speak or act without thinking about possible consequences. They act without forethought or planning, but also with an absence of malice. A child with ADHD will shout out in order to be attended to, or will butt into conversation and show an inability to wait their turn.
In addition, to the three core factors there are a number of additional features which may be present. Most children with ADHD need to have what they want when they want it. They are unable to show gratification, being unable to put off the receipt, of something that they want, for even a short period. Linked to this they also show "temporary myopia", where they have a lack of awareness or disregard for time - they live for the present, where what has gone before or what might be to come is of little consequence.
They may show insatiability, going on and on about a particular topic or activity, not letting the matter drop, with constant interrogation until they receive what is an acceptable response to them. Frequently they have a social clumsiness where they are over-demanding, bossy, over-the-top and loud. They misread facial expression and other social cues. Consequently even when they are trying to be friendly their peers can isolate them.
Sometimes there is also a physical clumsiness, occasionally because of their impulsivity, but also perhaps because of poor co-ordination. Some of these problems may be related to developmental dyspraxia, which is a specific learning difficulty sometime seen alongside ADHD. These children will also be dis-organised and experience problems with planning, tidiness and have the right equipment for a task.
As well as the developmental dyspraxia, many other difficulties can be present in children with ADHD. These include other specific learning difficulties e.g. dyslexia, Autistic Spectrum Disorders, Oppositional Defiant Disorder, Conduct Disorder, etc.
At Primary School age up to 50% of children with ADHD will have additional problems of oppositional defiant behaviour. About 50% of children with ADHD will experience specific learning difficulties. Many will have developed low self-esteem in relation to school and their social skills. By late childhood children with ADHD who have not developed some co-morbid psychiatric, academic or social disorder will be in the minority. Those who remain as having purely ADHD are likely to have the best outcome in relation to future adjustment.
Additionally some professionals suggest that any primary age child who has developed Oppositional Defiant Disorder or Conduct Disorder will have ADHD as the primary problem, even if this is not immediately evident from their behaviour. At present, a diagnosis of ADHD is usually determined through referral to DSM IV criteria. (Appendix 1) There are three types of ADHD recognised: - ADHD predominantly hyperactive/impulsive; ADHD predominantly inattentive; ADHD combined. The ADHD predominantly inattentive is what used to be referred to as ADD (Attention Deficit Disorder without the hyperactivity).
Generally, it is considered that there are five times as many boys than girls who show ADHD (HI), compared with twice as many boys to girls who show ADHD (I). It is recognised that around 5% of children are affected by ADHD, with perhaps about 2% experiencing severe problems. It should also be noted that some children will show aspects of an attentional deficit, which, although significant from their point of view, would not trigger a diagnosis of ADHD. There is a continuum of severity of problems in such a way that some children will have an attentional deficit but will not be ADHD. Yet others will show attention problems but for other reasons, for example, daydreaming/inattention because of something on their mind e.g. family bereavement.
ADHD - Probable Causes
It is generally agreed that there is a biological predisposition to the development of ADHD, with hereditary factors playing the most significant part. It is likely to be the genetic transmission which results in dopamine depletion or under-activity in the prefrontal - striatal - limbic regions of the brain which are known to be involved in behavioural disinhibition, which is considered to be most significant in ADHD, sensitivity to behavioural consequences and differential reward. Dopamine is a neurotransmitter, which facilitates the action of neurones by allowing passage of messages across the synaptic gaps between neurones. The condition is made worse by perinatal complications, toxins, neurological disease or injury, and dysfunctional child rearing. Poor parenting doesn't itself cause ADHD.
In looking at potential predictors of ADHD there are several factors, which are found to be predicative of ADHD. These include: -
- a family history of ADHD
- maternal smoking and alcohol consumption during pregnancy
- single parenthood and low educational attainment
- poor infant health and developmental delay
- early emergence of high activity and demanding behaviour in infancy
- critical/directive maternal behaviour in early infancy
As baby's children with ADHD tend to be colicky, difficult to settle, failing to sleep through the night and show delayed development. Parents will make comments, which reflect aspects of the ADHD - "He never walks, he runs", "I can't turn my back for a minute", "The terrible two's just seemed to go on forever". Parents often feel embarrassed about taking their child anywhere. The young child with ADHD is more accident-prone, probably because of the high speed of movement, lack of caution, over-activity and inquisitiveness. Often they have relatively more files at the Accident and Emergency Unit. Toilet training is often difficult which many children not bowel-trained until after three years and they continue to have accidents long after their peers do not. There is also found a strong association between ADHD and enuresis. There is the suggestion that ADHD should not be diagnosed in a child under the age of three years, perhaps the term 'at risk of ADHD' is more appropriate.
Diagnosis is usually made once the child is at school, where sitting appropriately, attending to directed activities and turn taking are expected of all children.
Impact of Children with ADHD on School Staff
Within the UK, there has been a gradual increase in the number of children diagnosed as having ADHD. Many of these children will be prescribed medication, to such an extent that it has been suggested that the 3R's are now made up of reading, writing and Ritalin.
There is the recognition that there is therefore the need to increase staff awareness about ADHD and it's implications. To this end Lennon Swart, Consultant Clinical Psychologist, and myself (Peter Withnall) were commissioned by a Multi-Agency Working Group in Durham to produce an information leaflet for teachers, proving awareness raising details covering diagnosis, associated disorders, causes, possible classroom strategies, medication and possible side effects of medication.
Once teachers are aware of ADHD and it management they are in an ideal position to help in the assessment, diagnosis and monitoring of pupils with ADHD in their schools. All too often, however, the first that they hear of any child with ADHD being diagnosed and treated is from the parent, sometimes even from the child, with an envelope with medication. This is not a satisfactory approach and does not encourage school staff "on board" in a child's treatment.
There are also other effects on staff, which can make things more difficult if they are not aware of them. For example, off task and inappropriate behaviour has an effect on shaping a teacher's behaviour, over time students who perform badly are praised less and criticised more. Teachers tend to take appropriate behaviour for granted and therefore provide low rates of positive reinforcement even when the child with ADHD is behaving appropriately. In terms of rating the performance and behaviour of children with ADHD it is likely that the ADHD provides a negative halo effect in terms of a teacher's perceptions, where the children are seen as worse than they actually are.
However, adults who had been hyperactive as children report that a teacher's caring attitude, extra attention and guidance were the turning point in helping them overcome their childhood problems. Also, if teachers perceive that their opinions are sought, respected and valued and that their input is important in the process they will be advocated in the child's treatment and management.
Teaching staff are often the first people to express concern about children who have or may have ADHD. Many professionals feel that school is the optimal place in which to diagnose ADHD, with some clinician suggesting that school impairment must be an essential component if the diagnosis is to be made.
To this end it is helpful if school staff monitor and record a child's behaviour once a concern has been expressed. Frequently they will be asked to complete a questionnaire or rating scale to provide the clinician with quantitative information. The most frequently used rating scale is the Connors Teacher Rating Scale, the short version of which consists of 28 items to be rated on a four-point scale. Quantitative information is then calculated in relation to four factors - oppositional, cognitive problems/inattention, hyperactivity, ADHD in - the raw scores from the ratings having had the age of the child taken into account. The ADHD index provides an indication of the 'risk of ADHD'.
Re-administration of this scale may also be carried out in order to assess the effects of any treatment / management strategy. A shortened version, of ten items, call the Iowa-Connors Rating Scale may also be used to monitor treatment effects.
ADHD in the Classroom
Children with ADHD have problems with their cognitive processes in terms of working memory, temporal myopia and the associated difficulties of disorganisation and poor planning, as well as the behavioural aspects involving impulsivity, inattention and over activity. Many children with ADHD also have problems with social interaction and social rejection because of their behaviour and poor social skills. This, along with the likelihood of aspects of specific learning difficulties, results in failure within the classroom and a low self-esteem. This all results in a downward spiral for the child.
'Self-esteem is like a rain forest - once you chop it down it takes forever to grow back' Barbara Stein (1994)
| Model Pupil | ADHD | Reframing |
| 1. Sits still | Fidgets | Animated |
| 2. Attends | Distracted | Aware |
| 3. Obeys requests | Disregards rules | Individual |
| 4. Co-operative | Disruptive | Enthusiastic |
| 5. Organised | Disorganised | Original |
| 6. Aware of others | Peer problems | Intense |
Intervention Strategies
It is recognised that multi-modal responses to the management of ADHD are the most appropriate and beneficial. However, by far the most effective single approach is that involving medication.
Use of ADHD Stimulant Medication During School Hours
Drug therapy can be an integral part of treatment but show not be considered the only treatment for ADHD. However, it has been found that it is effective in up to 90& of the children diagnosed as having ADHD. It is important that there is a diagnostic evaluation before starting treatment and for continued monitoring during treatment. The drugs commonly used are Methylphenidate (Ritalin) and Dexamphetamine (Dexedrine). These are psycho stimulants. They have what might be considered a "paradoxical effect" in that they "calm the child down", but do so by stimulating the inhibitory mechanisms, thus providing the child with the ability to stop and think before acting.
Stimulant medication was first prescribed for children in 1937, with this increasing signification in the 1950's when Ritalin was released for used in 1954. It is reportedly one of the safest paediatric drugs in current use.
Dosage and frequency requirements are highly individual and depend only in part on the size and age of the child. Indeed, it is often found that higher doses are required for younger, smaller children that are needed for older adolescents. Each dose provides improved attention for about four hours. Both drugs act within thirty minutes and the effects peak after about one and a half hours for Dexamphetamine and after about two hours for Methylphenidate. The Methylphenidate appears less likely to produce any unwanted side effects so this is generally the first choice. The effectiveness of the medication can be monitored with the use of behaviour rating scales and side-effect rating scales completed by teachers and parents, in addition to home-based and classroom observation. The usual mode of application consists of three doses, four houses apart, e.g. 8am, 12 noon and 4pm. Variations do occur, in order to meet the individual student's needs. Some psychiatrists recommend a mid-morning dose, for example, so that the pupil's attention and concentration are not impaired for the last hour of morning school but also to help their impulse control during the less structured lunch break.
The beneficial effects are often noted from the first day of use of medication. The behavioural effects are well documented and are:
- reduction in classroom disruption
- increase in on-task behaviour
- increased compliance with teacher requests
- decrease in aggression
- increase in appropriate social interaction
- reduction in conduct problems
Children are generally calmer, less restless, less impulsive, less insatiable and more reflective. They can complete work without supervision, are more settled, more organised, with neater writing and presentation.
Children with hyperactivity tend to respond more consistently to stimulant medication than those without. What must be noted is that if a child in unresponsive to one of the psycho stimulants it is still reasonable to try another, as they tend to work in slightly different ways. It has been reported that up to 90% of children with ADHD respond well to one of these forms of medication.
Possible Side Effect of ADHD Medication
The vast majority of people have no significant side effects from Ritalin; however, the unwanted effects of psycho stimulants may include initial insomnia (especially with a late afternoon dose), suppression of appetite and depression of mood. These can usually be avoided by careful attention to the dosage and its timing. Other common side effects are weight-loss, irritability, abdominal pain, headaches, drowsiness and a proneness to crying. Motor tics are a rare side-effect but do occur in a very small proportion of children being treated with medication.
Some children experience what has been termed a "rebound effect" in the evenings, when their behaviour appears to deteriorate markedly. This may be a perceived deterioration in that it may simply be a return to the previous behaviour pattern evident prior to use of medication, once the effects of the afternoon dose have worn off. Also occasionally children who are in effect receiving too high a dose can show what is termed a "Zombie state", where they show cognitive over focussing, blunting of emotional response or social withdrawal.
Consequently, although many of the most serious possible side effects are rare, their potential impact means that children on medication should be monitored very carefully. This monitoring is necessary in relation to the beneficial effects as well as the unwanted effects. If the medication is not having the desired effect then there is no point in continuing with this course of action, bearing in mind the previous comment in relation to the possible use of other psycho stimulant medication. Information from school concerning the monitoring must be made available to the person prescribing the medication. It needs to be realised that school staff can provide essential, critical, objective information on the child's response to the medication and any other interventions. A monitoring form is included later.
It must be remembers that individual children differ in their response to medication, with increased variation and lack of predictability more evident with children who have recognised neurological damage.
Medication is seen as one component of intensive long-term treatment of ADHD. It must be remembered that this is a chronic disorder for which no short-term treatment is sufficient or effective, although at times the effects of medication can be almost magical.
Classroom Organisation and the ADHD Child
There are many aspects of classroom organisation, which can make a difference to the way in which children with ADHD behave. In this section some simple suggestions will be made which have been found to provide, in effect, increased structure, which has then had a positive effect on behaviour.
- Placement of the child so that distractions can be minimised
- Classrooms relatively free from extraneous auditory and visual stimuli are desirable - complete removed of distractions is not warranted.
- Seating between positive role models
- Preferable those who the child sees as significant others, this encourages peer tutoring and co-operative learning.
- Seating in rows or U-shape rather than clusters
- Among children with behavioural problems on-task behaviour doubles as conditions are changed from desk clusters to rows - rates of disruption are three times higher in clusters.
Provision of structure to lessons and routine to the day
Within a consistent routine the child will function significantly better when provided with multiple shortened work periods, opportunities for choice among work activities and enjoyable reinforcers.
- Regular breaks/changes in activity - within understood routine - Interspersing academic seated activities with those that require movement diminishes fatigue and wandering.
- General calmness - Sometimes easier said than done, this reduces the likelihood of any over reaction to a situation.
- Avoiding unnecessary change - Keep informal changes to a minimum, provide additional structure during transition periods.
- Preparation for change - Mention the time remaining, time countdown and advance warning and indicate what is expected and appropriate
- Allow the child to change work sites frequently - Provide some variation for the child and reduces the likelihood of inattention.
- Traditional closed classroom - Noisy environments are association with less task attention and a higher rate of negative comments among hyperactive children. Opportunities for these are less within a closed classroom that with an open plan arrangement.
- Academic activities in the morning - It is recognised that there is generally a progressive worsening of a child's activity levels and inattention over the course of the day.
- Orderly routines for storing and accessing materials - Easy access reduces the effects of the child's disorganisation - perhaps colour coding could facilitate access e.g. all materials, books, worksheets etc. in relation to maths could be indicated by the colour 'blue' - blue signs, blue containers etc.
- Appropriate Curriculum Presentation - Varied presentation of tasks to maintain interest. Use of different modalities increases novelty/interest which enhance attention and reduced activity level
- Child to repeat directions given - Compliance in the classroom is increased when the child is required to repeat directions / instructions
- Removal of extraneous information - For example, from published work sheets or other documents, so that all the detail is relevant to the task, perhaps also reducing the amount of information per page
- High novelty of learning tasks
- Short spells on one topic, operating within the child's limit of concentration. Assignments should be brief, feedback immediate; short time limits for task completion; perhaps use of a timer for self monitoring
- Provision of tasks of appropriate duration where the start and end point are clearly defined
There are three key goals for any child in a classroom setting:
- to start when everyone else does
- to stop when every one else does and
- to focus on the same things as the other children
Consistency of management and expectation
- Clear, concise instruction which appear specific to the child
- Maintain eye contact with the child; compliance and task completion increase when simple, single directions are given
- Short sequences of instructions
- Minimal repetitive drill exercises
- Again to reduce the likelihood of inattention and boredom
- Active participation throughout the lesson
- Low level of controlling language
- Tasks appropriate to the child's level of ability
- Assignments in small chunks
- Alternate sitting and standing
- Provide documents with large print
This, as well as giving less information per page, allows for easier access to the information.
Behaviour Management
General points:
- Develop a workable set of rules in the classroom
- Respond consistently and quickly to inappropriate behaviour
- Structure the classroom activities to minimise disruption
- Respond to, but do no become angry with, inappropriate behaviour
Despite the substantial success of teacher administered behaviour management programmes there is little evidence that treatment gains persist once the programmes are terminated. Also the improvement produced by contingency management in one setting do not generalise to settings where the programmes are not in effect. The fact that most behaviour management strategies are based on consequences means that they are not as effective with children with ADHD as they would be with children who are aware of, and concerned about, consequence.
There are several strategies which are considered to be effective with children with ADHD.
Continuous reinforcement
It has been found that children with ADHD perform as well as non-ADHD children when provided with continuous reinforcement - that is when they are rewarded every time they do what is expected of them - they perform significantly worse with partial reinforcement.
Token Economy
In this strategy there is set up a menu of rewards, which the child can purchase with tokens that he or she earns for agreed appropriate behaviour. With young children (y - 7 years) that tokens need to be tangible - counters, beads, buttons etc - the menu of rewarding items needs to be changed regularly to provide novelty and avoid habituation. For older children the tokens can be points, starts, ticks on a chart etc. Under this system there is not cost to the child if they behave inappropriately, other then not being rewarded.
Response Cost
This is the loss of a reinforcer / token contingent on inappropriate behaviour. If a child misbehaves he of she not only does not get rewarded but they also have something taken from them - it costs them if they respond in an inappropriate way. Empirical findings suggest that response cost may be the most powerful means of managing the consequence for children with ADHD or other disruption behavioural problems.
However, in the traditional model of response cost many children would be bankrupt very rapidly. It is recommended that one or two bits of behaviour that the child does reliably are also included in order to make it more likely that the child will succeed.
In another variation, which appears to be particularly, useful for children with ADHD the child is initially provided with the maximum number of points or tokens to be earned during the whole day. The child must then work through the whole day to retain those reinforcers. It has been found that impulsive children who better to keep their plates full rather than to refill an empty place.
Using a similar approach for the management of attention-demanding behaviour it is sometimes useful to provide a child with a specific number of 'cards' that can then be spent by the child to purchased immediate adult attention. The aim is to give the child the cards at the beginning of the day so that he or she learns to spend them wisely, the idea would be to work towards reducing the number of cards available to the child over time.
Highway Patrol Method
- Identify the offence - the inappropriate behaviour
- Inform the offender of the punishment - the response cost
- Remain polite and businesslike - stay calm and objective
Self-monitoring
It is possible to improve a child's concentration and application to task by means of self-monitoring. Here the child takes some responsibility for the actual management of his or her behaviour.
Timers
Use of a kitchen time, egg timer, stop watch or clock can provide a structured way of letter the child know what the task expectations are in terms of the length of time that he or she is required to work. The actual length of time used initially needs to be within the child's capabilities and the time would be extended imperceptibly.
Visual Cues
Having visual cues around the room, depicting a message to the child in terms of behavioural expectations can facilitate improvements in self-control. Specific reminders, non-verbal cues from adults can aid the child's awareness of and response to the visual cues.
Auditory Cues
Occasionally taped auditory cues have been used to remind students of expected behaviour. The cues can consist of bleeps produced at varying times during the lesson. These can be simply reminders to the child or they can be a cue to the child to record whether he or she was on-task at the time of the bleep. Such approaches are useful for children with ADHD who are not showing Oppositional Defiant or Conduct Disorder. Tape-recorded cues of reminders to 'get on with your work', 'do your best' etc. have been found helpful, particularly it the cues are recorded using the child's father's voice.
Student Involvement
It is evident that gaining parental and student co-operation is crucial.
It is not sufficient to assess, diagnose, prescribe and monitor. Sam is an eight-year-old boy who has been diagnosed as have ADHD. He has been prescribed medication and his mother gives it to him as required. Little change in his behaviour was noted either at home or at school. It turned out that Sam was taking his medication, keeping it under his tongue until his mother had gone and then spitting it out. The child needs to be involved and 'on board' in terms of the treatment approach taken.
Old children (7+) should be included during meetings to help set goals and determine appropriate rewards. Involving children in this way often enhances their motivation to participate and be successful in their programme.
Home-school notes are also seen to be beneficial - they need to be clear and accurate but not necessarily very specific. Use of such notes has been found to improve classroom conduct and academic performance of students of all ages - with older students the manner of presenting the note and their active involvement in its use are critical.
Staged Assessment Procedures and Co-morbidity.
There is no need for the initiation of a statutory assessment of special educational needs simply because a child has a diagnosis of ADHD. It depends on the nature and severity of the individual child's difficulties and how they impact on his learning and ability to access the curriculum.
Generally, it is the child with a multiplicity of problems who presents with sufficient difficulties to require resources, which are additional to or different from those normally available. For some children there is the need for the protection of a Statement, for others medication alone is the answer. For others a combinations is required.
It has been found that:
- 45% of those diagnosed ADHD will also have O.D.D.
- 25% - Conduct Disorder
- 25% - anxiety disorders
- 50% - specific learning difficulties
- 70% - depression
- 20% - bipolar disorder
- 50% - sleep problems
- 31% - social phobias
Adult Outcome
Some children mature in ways that cause the ADHD symptoms to reduce. For others, hyperactivity might diminish, particularly in adolescence, but problems with impulsivity, in attention and organisation continue.
There is some dispute about the proportion of children for whom maturation is the "cure" - most believe that one third to one half of the ADHD population will continue to have ADHD symptoms as adults. Some researchers have suggested that only one third of the ADHD population will outgrow the disorder.
Untreated adults who experience multiple symptoms are most likely to engage in serious antisocial behaviour and/or drug and alcohol abuse. A long-term study found that those who were diagnosed with ADHD as children are, compared to the general population, "disproportionably uneducated, under-employed and plagued by mental problems" and by their early twenties are "twice as likely to have an arrest record, five times as likely to have a felony conviction and nine times as likely to have served time in prison".
Some research carried out in 1984 shoed that children with ADHD who are treated with psycho stimulant medication generally have a better adult outcome. Two groups of adults were compared, one group had been treated with Ritalin for a least three years at primary school age and the other group, similarly diagnosed as ADHD, had received no medication. The adults who were given Methylphenidate as children, had less psychiatric treatment, fewer car accidents, more independence and were less aggressive.
However, it has also been found that "most prosperous entrepreneurs have ADHD" - high energy levels, intensity about ideas and relationships, affinity to stimulating environments.
Conclusion
ADHD is turning out to be a significant factor in the lives of a very large proportion of the general population. Not only do we have a relatively high number of children diagnoses with ADHD, perhaps between 5% and 7% of the population, but we also have the ripple effect where these children and their behaviour touch the lives of a much greater proportion of the population.
It is recognised that children with ADHD who are undiagnosed or untreated are likely not only to struggle through their school years but also to underachieve as adults. They are more likely to show deviant, antisocial behaviour and to end up on prison.
It is therefore vitally important that we do all we can to aid accurate diagnosis of children with ADHD, the help to monitor treatment effects and to provide consistent management strategies to facilitate their impulse control and application to task. In this way perhaps we can help to minimise the detrimental effects of the condition and improve the likely outcome for children with ADHD.
Appendix 2
| Child: | Name of Teacher |
| Date: | Day: |
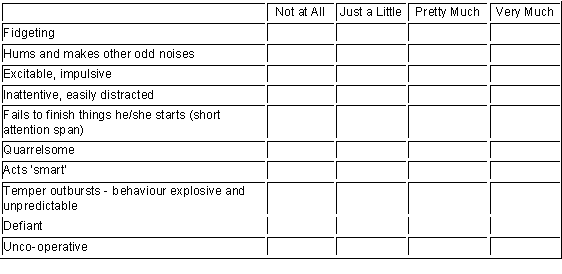
The IOWA Connors Teacher's Rating Scale
Check the column which best describes this child today.
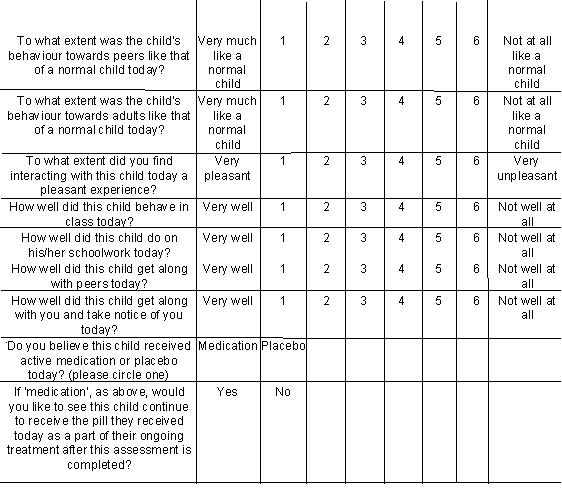
Please circle relevant number - 1 being highest score and 6 being lowest score.
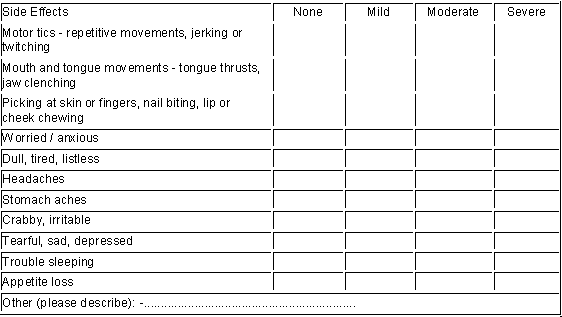
Appendix 3
A Rating Scale for Common Stimulant Side-effects
About the author: Peter Withnall is Area Senior Educational Psychologist, County Durham.
APA Reference
Staff, H.
(2008, December 17). Supporting an ADHD Child in the Classroom, HealthyPlace. Retrieved
on 2026, May 14 from https://www.healthyplace.com/adhd/articles/supporting-an-adhd-child-in-the-classroom

