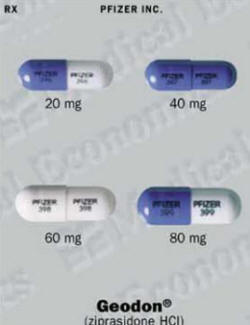
Geodon (Ziprasidone HCl) Patient Information
Find out why Geodon is prescribed, side effects of Geodon, Geodon warnings, effects of Geodon during pregnancy, more - in plain English.
Generic name: Ziprasidone hydrochloride
Brand name: Geodon
Pronounced: GEE-oh-dahn
Geodon Prescribing Information
Why is this drug prescribed?
Geodon is used in the treatment of the crippling mental disorder known as schizophrenia. Researchers believe that it works by opposing the action of serotonin and dopamine, two of the brain's major chemical messengers. Because of its potentially serious side effects, Geodon is typically prescribed only after other medications have proved inadequate.
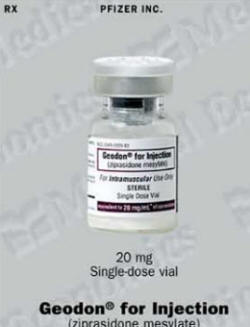
Geodon is usually taken in capsule form. An injectable version is available for quick relief of agitated patients. Injectable Geodon is generally used for no more than a few days.
Most important fact about this drug
In some people with heart problems or a slow heartbeat, Geodon can cause serious and potentially fatal heartbeat irregularities. The chance of a problem is greater if you are taking a water pill (diuretic) or a medication that prolongs a part of the heartbeat known as the QT interval. Many of the drugs prescribed for heartbeat irregularities prolong the QT interval and should never be combined with Geodon. Other drugs to avoid when taking Geodon include Anzemet, Avelox, Halfan, Inapsine, Lariam, Mellaril, Nebupent, Orap, Orlaam, Pentam, Probucol, Prograf, Serentil, Tequin, Thorazine, Trisenox, and Zagam. If you're uncertain about the risks of any drug you're taking, be sure to check with your doctor before combining it with Geodon.
How should you take this medication?
Geodon capsules should be taken twice a day with food.
--If you miss a dose...
Why is this drug prescribed?
Geodon is used in the treatment of the crippling mental disorder known as schizophrenia. Researchers believe that it works by opposing the action of serotonin and dopamine, two of the brain's major chemical messengers. Because of its potentially serious side effects, Geodon is typically prescribed only after other medications have proved inadequate.
Geodon is usually taken in capsule form. An injectable version is available for quick relief of agitated patients. Injectable Geodon is generally used for no more than a few days.
Most important fact about this drug
In some people with heart problems or a slow heartbeat, Geodon can cause serious and potentially fatal heartbeat irregularities. The chance of a problem is greater if you are taking a water pill (diuretic) or a medication that prolongs a part of the heartbeat known as the QT interval. Many of the drugs prescribed for heartbeat irregularities prolong the QT interval and should never be combined with Geodon. Other drugs to avoid when taking Geodon include Anzemet, Avelox, Halfan, Inapsine, Lariam, Mellaril, Nebupent, Orap, Orlaam, Pentam, Probucol, Prograf, Serentil, Tequin, Thorazine, Trisenox, and Zagam. If you're uncertain about the risks of any drug you're taking, be sure to check with your doctor before combining it with Geodon.
How should you take this medication?
Geodon capsules should be taken twice a day with food.
--If you miss a dose...
Take it as soon as you remember. If it is almost time for your next dose, skip the one you missed and go back to your regular schedule. Do not take 2 doses at once.
--Storage instructions...
Store at room temperature.
What side effects may occur?
Side effects cannot be anticipated. If any develop or change in intensity, inform your doctor as soon as possible. Only your doctor can determine if it is safe for you to continue taking Geodon.
-
More common side effects may include: Accidental injury, cold symptoms, constipation, cough, diarrhea, dizziness, drowsiness, dry mouth, indigestion, muscle tightness, nausea, rash, stuffy and runny nose, upper respiratory infection, vision problems, weakness
-
Other side effects may include: Abdominal pain, abnormal body movements, abnormal ejaculation, abnormal secretion of milk, abnormal walk, abnormally low cholesterol, agitation, amnesia, anemia, bleeding gums, bleeding in the eye, blood clots, blood disorders, blood in urine, body spasms, breast development in males, bruising or purple spots, cataracts, chest pain, chills, clogged bowels, confusion, conjunctivitis (pinkeye), coordination problems, decreased blood flow to the heart, delirium, difficulty breathing, difficulty swallowing, difficulty with orgasm, double vision, dry eyes, enlarged heart, eyelid inflammation, female sexual problems, fever, flank pain, flu-like symptoms, fungal infections, gout, hair loss, heavy menstruation, heavy uterine or vaginal bleeding, high blood pressure, high blood sugar, hives, hostility, impotence, increased reflexes, increased sensitivity to touch or sound, inflammation of the cornea, inflammation of the heart, involuntary or jerky movements, irregular heartbeat, liver problems, lockjaw, loss of appetite, loss of menstruation, low blood sugar, low blood pressure, low body temperature, lymph disorders, male sexual problems, muscle disorders, muscle pain, muscle weakness, nighttime urination, nosebleed, pneumonia, prickling or tingling sensation, rapid heartbeat, rectal bleeding, rigid muscle movement, ringing in ears, rolling of the eyeballs, sensitivity to sunlight, skin problems, slow heartbeat, slowed movement, speech problems, stroke, sudden drop in blood pressure upon standing up, swelling in the arms and legs, swelling in the face, swollen lymph nodes, swollen tongue, tarry stools, tendon inflammation, thirst, throat spasms, thyroid disorders, tremor, twitching, uncontrolled eye movement, urination decrease or increase, vaginal bleeding, vein inflammation, vertigo, vision disorders, vomiting, vomiting or spitting blood, yellowed skin and eyes, weight gain, white spots in the mouth
Why should this drug not be prescribed?
Do not take Geodon if you have the heartbeat irregularity known as QT prolongation, have had a recent heart attack, or suffer from heart failure. You'll also need to avoid this drug if it gives you an allergic reaction.
Special warnings about this medication
Remember that Geodon can cause dangerous--even fatal--heartbeat irregularities. Warning signs include dizziness, palpitations, and fainting. Tell your doctor immediately if you experience any of these symptoms. Be careful to avoid drugs that prolong the QT interval of the heartbeat. Check with your doctor before combining any other medication with Geodon.
Particularly during the first few days of therapy, Geodon can cause low blood pressure, with accompanying dizziness, fainting, and rapid heartbeat. Tell your doctor if you experience any of these side effects. To minimize such problems, your doctor will increase your dose gradually. If you are prone to low blood pressure, take blood pressure medicine, become dehydrated, or have heart disease or poor circulation in the brain, use Geodon with caution.
Geodon may cause drowsiness and can impair your judgment, thinking, and motor skills. Use caution while driving and don't operate potentially dangerous machinery until you know how this drug affects you.
 Geodon poses a very slight risk of seizures, especially if you are over age 65, have a history of seizures, or have Alzheimer's disease.
Geodon poses a very slight risk of seizures, especially if you are over age 65, have a history of seizures, or have Alzheimer's disease.
Drugs such as Geodon sometimes cause a condition called Neuroleptic Malignant Syndrome. Symptoms include high fever, muscle rigidity, irregular pulse or blood pressure, rapid heartbeat, excessive perspiration, and changes in heart rhythm. If these symptoms appear, tell your doctor immediately. You'll need to stop taking Geodon while the condition is under treatment.
There also is the risk of developing tardive dyskinesia, a condition marked by slow, rhythmical, involuntary movements. This problem is more likely to occur in mature adults, especially older women. When it does, use of Geodon is usually stopped.
Geodon can suppress the cough reflex; you may have trouble clearing your airway. Some people taking Geodon also develop a rash. Tell your doctor when this happens. If the rash doesn't clear up with treatment, you may have to discontinue the drug.
Other antipsychotic medications have been known to interfere with the body's temperature-regulating mechanism, causing the body to overheat. Although this problem has not occurred with Geodon, caution is still advisable. Avoid exposure to extreme heat, strenuous exercise, and dehydration. There also is a remote chance that this medication may cause abnormal, prolonged and painful erections.
Possible food and drug interactions when taking this medication
 Remember that you must never combine Geodon with any drug that prolongs the part of the heartbeat known as the QT interval (see "Most important fact about this drug"). Check with your doctor or pharmacist if you have any doubts about a drug you're taking.
Remember that you must never combine Geodon with any drug that prolongs the part of the heartbeat known as the QT interval (see "Most important fact about this drug"). Check with your doctor or pharmacist if you have any doubts about a drug you're taking.
If Geodon is taken with certain other drugs, the effects of either could be increased, decreased, or altered. It is especially important to check with your doctor before combining Geodon with the following: Carbamazepine (Tegretol) Certain blood pressure medications Drugs that boost the effects of dopamine such as Mirapex, Parlodel, Permax, and Requip Drugs that affect the brain and nervous system, such as sedatives, tranquilizers, and antidepressants Ketoconazole (Nizoral) Levodopa (Larodopa, Sinemet)
Special information if you are pregnant or breastfeeding
Geodon has caused fetal harm when tested in animals. It should be taken during pregnancy only if the benefits outweigh the potential risk. Notify your doctor as soon as you become pregnant or plan to become pregnant.
It is not known whether Geodon appears in breast milk, and breastfeeding is not recommended.
Recommended dosage
GEODON CAPSULES
The usual starting dose is 20 milligrams twice a day. If needed, the dosage may be increased at several-week intervals up to a maximum of 80 milligrams twice a day.
Overdosage
Any medication taken in excess can have serious consequences. If you suspect an overdose, seek medical help immediately.
Symptoms of Geodon overdose may include: Drowsiness, slurred speech, high blood pressure
Geodon Prescribing Information
Detailed Info on Signs, Symptoms, Causes, Treatments of Schizophrenia
APA Reference
Staff, H.
(2009, January 3). Geodon (Ziprasidone HCl) Patient Information, HealthyPlace. Retrieved
on 2026, March 28 from https://www.healthyplace.com/other-info/psychiatric-medications/geodon-ziprasidone-patient-information