Avandia for Treatment of Diabetes - Avandia Full Prescribing Information
Brand Name: AVANDIA
Generic Name: rosiglitazone maleate
Contents:
Indications and Usage
Dosage and Administration
Dosage Forms and Strenghts
Contraindications
Warnings and Precautions
Adverse Reactions
Drug Interactions
Use in Specific Populations
Overdosage
Description
Clinical Pharmacology
Nonclinical Toxicology
Clinical Studies
How Supplied
Avandia, rosiglitazone maleate, patient information (in plain English)
WARNING
CONGESTIVE HEART FAILURE AND MYOCARDIAL ISCHEMIA
- Thiazolidinediones, including rosiglitazone, cause or exacerbate congestive heart failure in some patients [see WARNINGS AND PRECAUTIONS]. After initiation of AVANDIA, and after dose increases, observe patients carefully for signs and symptoms of heart failure (including excessive, rapid weight gain, dyspnea, and/or edema). If these signs and symptoms develop, the heart failure should be managed according to current standards of care. Furthermore, discontinuation or dose reduction of AVANDIA must be considered.
- AVANDIA is not recommended in patients with symptomatic heart failure. Initiation of AVANDIA in patients with established NYHA Class III or IV heart failure is contraindicated. [See CONTRAINDICATIONS and WARNINGS AND PRECAUTIONS.]
- A meta-analysis of 42 clinical studies (mean duration 6 months; 14,237 total patients), most of which compared AVANDIA to placebo, showed AVANDIA to be associated with an increased risk of myocardial ischemic events such as angina or myocardial infarction. Three other studies (mean duration 41 months; 14,067 total patients), comparing AVANDIA to some other approved oral antidiabetic agents or placebo, have not confirmed or excluded this risk. In their entirety, the available data on the risk of myocardial ischemia are inconclusive. [See WARNINGS AND PRECAUTIONS.]
Indications and Usage
Monotherapy and Combination Therapy
AVANDIA is indicated as an adjunct to diet and exercise to improve glycemic control in adults with type 2 diabetes mellitus.
Important Limitations of Use
- Due to its mechanism of action, AVANDIA is active only in the presence of endogenous insulin. Therefore, AVANDIA should not be used in patients with type 1 diabetes mellitus or for the treatment of diabetic ketoacidosis.
- The coadministration of AVANDIA and insulin is not recommended.
- The use of AVANDIA with nitrates is not recommended.
Dosage and Administration
The management of antidiabetic therapy should be individualized. All patients should start AVANDIA at the lowest recommended dose. Further increases in the dose of AVANDIA should be accompanied by careful monitoring for adverse events related to fluid retention [see Boxed Warning and WARNINGS and PRECAUTIONS].
AVANDIA may be administered at a starting dose of 4 mg either as a single daily dose or in 2 divided doses. For patients who respond inadequately following 8 to 12 weeks of treatment, as determined by reduction in fasting plasma glucose (FPG), the dose may be increased to 8 mg daily as monotherapy or in combination with metformin, sulfonylurea, or sulfonylurea plus metformin. Reductions in glycemic parameters by dose and regimen are described under Clinical Studies . AVANDIA may be taken with or without food.
The total daily dose of AVANDIA should not exceed 8 mg.
Monotherapy
The usual starting dose of AVANDIA is 4 mg administered either as a single dose once daily or in divided doses twice daily. In clinical trials, the 4-mg twice-daily regimen resulted in the greatest reduction in FPG and hemoglobin A1c (HbA1c).
Combination With Sulfonylurea or Metformin
When AVANDIA is added to existing therapy, the current dose(s) of the agent(s) can be continued upon initiation of therapy with AVANDIA.
Sulfonylurea: When used in combination with sulfonylurea, the usual starting dose of AVANDIA is 4 mg administered as either a single dose once daily or in divided doses twice daily. If patients report hypoglycemia, the dose of the sulfonylurea should be decreased.
Metformin: The usual starting dose of AVANDIA in combination with metformin is 4 mg administered as either a single dose once daily or in divided doses twice daily. It is unlikely that the dose of metformin will require adjustment due to hypoglycemia during combination therapy with AVANDIA.
Combination With Sulfonylurea Plus Metformin
The usual starting dose of AVANDIA in combination with a sulfonylurea plus metformin is 4 mg administered as either a single dose once daily or divided doses twice daily. If patients report hypoglycemia, the dose of the sulfonylurea should be decreased.
Specific Patient Populations
Renal Impairment: No dosage adjustment is necessary when AVANDIA is used as monotherapy in patients with renal impairment. Since metformin is contraindicated in such patients, concomitant administration of metformin and AVANDIA is also contraindicated in patients with renal impairment.
Hepatic Impairment: Liver enzymes should be measured prior to initiating treatment with AVANDIA. Therapy with AVANDIA should not be initiated if the patient exhibits clinical evidence of active liver disease or increased serum transaminase levels (ALT >2.5X upper limit of normal at start of therapy). After initiation of AVANDIA, liver enzymes should be monitored periodically per the clinical judgment of the healthcare professional. [See WARNINGS and PRECAUTIONS and CLINICAL PHARMACOLOGY.]
Pediatric: Data are insufficient to recommend pediatric use of AVANDIA [see USE in SPECIFIC POPULATIONS].
Dosage forms and Strengths
Pentagonal film-coated TILTAB tablet contains rosiglitazone as the maleate as follows:
- 2 mg - pink, debossed with SB on one side and 2 on the other
- 4 mg - orange, debossed with SB on one side and 4 on the other
- 8 mg - red-brown, debossed with SB on one side and 8 on the other
Contraindications
Initiation of AVANDIA in patients with established New York Heart Association (NYHA) Class III or IV heart failure is contraindicated [see BOXED WARNING].
Warnings and Precautions
Cardiac Failure
AVANDIA, like other thiazolidinediones, alone or in combination with other antidiabetic agents, can cause fluid retention, which may exacerbate or lead to heart failure. Patients should be observed for signs and symptoms of heart failure. If these signs and symptoms develop, the heart failure should be managed according to current standards of care. Furthermore, discontinuation or dose reduction of rosiglitazone must be considered [see BOXED WARNING].
Patients with congestive heart failure (CHF) NYHA Class I and II treated with AVANDIA have an increased risk of cardiovascular events. A 52-week, double-blind, placebo-controlled echocardiographic study was conducted in 224 patients with type 2 diabetes mellitus and NYHA Class I or II CHF (ejection fraction ≤ 45%) on background antidiabetic and CHF therapy. An independent committee conducted a blinded evaluation of fluid-related events (including congestive heart failure) and cardiovascular hospitalizations according to predefined criteria (adjudication). Separate from the adjudication, other cardiovascular adverse events were reported by investigators. Although no treatment difference in change from baseline of ejection fractions was observed, more cardiovascular adverse events were observed following treatment with AVANDIA compared to placebo during the 52-week study. (See Table 1.)
Table 1. Emergent Cardiovascular Adverse Events in Patients With Congestive Heart Failure (NYHA Class I and II) Treated With AVANDIA or Placebo (in Addition to Background Antidiabetic and CHF Therapy)
| Events | AVANDIA N = 110 n (%) | Placebo N = 114 n (%) |
| Adjudicated | ||
| Cardiovascular deaths | 5 (5%) | 4 (4%) |
| CHF worsening | 7 (6%) | 4 (4%) |
| - with overnight hospitalization | 5 (5%) | 4 (4%) |
| - without overnight hospitalization | 2 (2%) | 0 (0%) |
| New or worsening edema | 28 (25%) | 10 (9%) |
| New or worsening dyspnea | 29 (26%) | 19 (17%) |
| Increases in CHF medication | 36 (33%) | 20 (18%) |
| Cardiovascular hospitalization* | 21 (19%) | 15 (13%) |
| Investigator-reported, non-adjudicated | ||
| Ischemic adverse events | 10 (9%) | 5 (4%) |
| - Myocardial infarction | 5 (5%) | 2 (2%) |
| - Angina | 6 (5%) | 3 (3%) |
| * Includes hospitalization for any cardiovascular reason. | ||
Initiation of AVANDIA in patients with established NYHA Class III or IV heart failure is contraindicated. AVANDIA is not recommended in patients with symptomatic heart failure. [See BOXED WARNING.]
Patients experiencing acute coronary syndromes have not been studied in controlled clinical trials. In view of the potential for development of heart failure in patients having an acute coronary event, initiation of AVANDIA is not recommended for patients experiencing an acute coronary event, and discontinuation of AVANDIA during this acute phase should be considered.
Patients with NYHA Class III and IV cardiac status (with or without CHF) have not been studied in controlled clinical trials. AVANDIA is not recommended in patients with NYHA Class III and IV cardiac status.
Myocardial Ischemia
Meta-Analysis of Myocardial Ischemia in a Group of 42 Clinical Trials
A meta-analysis was conducted retrospectively to assess cardiovascular adverse events reported across 42 double-blind, randomized, controlled clinical trials (mean duration 6 months).1
These studies had been conducted to assess glucose-lowering efficacy in type 2 diabetes, and prospectively planned adjudication of cardiovascular events had not occurred in the trials. Some trials were placebo-controlled and some used active oral antidiabetic drugs as controls. Placebo-controlled studies included monotherapy trials (monotherapy with AVANDIA versus placebo monotherapy) and add-on trials (AVANDIA or placebo, added to sulfonylurea, metformin, or insulin). Active control studies included monotherapy trials (monotherapy with AVANDIA versus sulfonylurea or metformin monotherapy) and add-on trials (AVANDIA plus sulfonylurea or AVANDIA plus metformin, versus sulfonylurea plus metformin). A total of 14,237 patients were included (8,604 in treatment groups containing AVANDIA, 5,633 in comparator groups), with 4,143 patient-years of exposure to AVANDIA and 2,675 patient-years of exposure to comparator. Myocardial ischemic events included angina pectoris, angina pectoris aggravated, unstable angina, cardiac arrest, chest pain, coronary artery occlusion, dyspnea, myocardial infarction, coronary thrombosis, myocardial ischemia, coronary artery disease, and coronary artery disorder. In this analysis, an increased risk of myocardial ischemia with AVANDIA versus pooled comparators was observed (2% AVANDIA versus 1.5% comparators, odds ratio 1.4, 95% confidence interval [CI] 1.1, 1.8). An increased risk of myocardial ischemic events with AVANDIA was observed in the placebo-controlled studies, but not in the active-controlled studies. (See Figure 1.)
A greater increased risk of myocardial ischemic events was observed in studies where AVANDIA was added to insulin (2.8% for AVANDIA plus insulin versus 1.4% for placebo plus insulin, [OR 2.1, 95% CI 0.9, 5.1]). This increased risk reflects a difference of 3 events per 100 patient-years (95% CI -0.1, 6.3) between treatment groups. [See WARNINGS AND PRECAUTIONS.]
Figure 1. Forest Plot of Odds Ratios (95% Confidence Intervals) for Myocardial Ischemic Events in the Meta-Analysis of 42 Clinical Trials
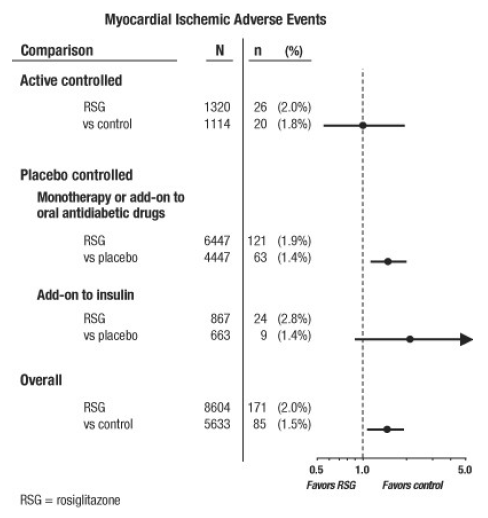
A greater increased risk of myocardial ischemia was also observed in patients who received AVANDIA and background nitrate therapy. For AVANDIA (N = 361) versus control (N = 244) in nitrate users, the odds ratio was 2.9 (95% CI 1.4, 5.9), while for non-nitrate users (about 14,000 patients total), the odds ratio was 1.3 (95% CI 0.9, 1.7). This increased risk represents a difference of 12 myocardial ischemic events per 100 patient-years (95% CI 3.3, 21.4). Most of the nitrate users had established coronary heart disease. Among patients with known coronary heart disease who were not on nitrate therapy, an increased risk of myocardial ischemic events for AVANDIA versus comparator was not demonstrated.
Myocardial Ischemic Events in Large Long-Term Prospective Randomized Controlled Trials of AVANDIA
Data from 3 other large, long-term, prospective, randomized, controlled clinical trials of AVANDIA were assessed separately from the meta-analysis. These 3 trials include a total of 14,067 patients (treatment groups containing AVANDIA N = 6,311, comparator groups N = 7,756), with patient-year exposure of 21,803 patient-years for AVANDIA and 25,998 patient-years for comparator. Duration of follow-up exceeded 3 years in each study. ADOPT (A Diabetes Outcomes Progression Trial) was a 4- to 6-year randomized, active-controlled study in recently diagnosed patients with type 2 diabetes naïve to drug therapy.
It was an efficacy and general safety trial that was designed to examine the durability of
AVANDIA as monotherapy (N = 1,456) for glycemic control in type 2 diabetes, with comparator arms of sulfonylurea monotherapy (N = 1,441) and metformin monotherapy (N = 1,454). DREAM (Diabetes Reduction Assessment with Rosiglitazone and Ramipril Medication, published report2) was a 3- to 5-year randomized, placebo-controlled study in patients with impaired glucose tolerance and/or impaired fasting glucose. It had a 2x2 factorial design, intended to evaluate the effect of AVANDIA, and separately of ramipril (an angiotensin converting enzyme inhibitor [ACEI]), on progression to overt diabetes. In DREAM, 2,635 patients were in treatment groups containing AVANDIA, and 2,634 were in treatment groups not containing AVANDIA.Interim results have been published 3 for RECORD (Rosiglitazone Evaluated for Cardiac Outcomes and Regulation of Glycemia in Diabetes), an ongoing open-label, 6-year cardiovascular outcomes study in patients with type 2 diabetes with an average treatment duration of 3.75 years. RECORD includes patients who have failed metformin or sulfonylurea monotherapy; those who have failed metformin are randomized to receive either add-on AVANDIA or add-on sulfonylurea, and those who have failed sulfonylurea are randomized to receive either add-on AVANDIA or add-on metformin. In RECORD, a total of 2,220 patients are receiving add-on AVANDIA, and 2,227 patients are on one of the add-on regimens not containing AVANDIA.
For these 3 trials, analyses were performed using a composite of major adverse cardiovascular events (myocardial infarction, cardiovascular death, or stroke), referred to hereafter as MACE. This endpoint differed from the meta-analysis' broad endpoint of myocardial ischemic events, more than half of which were angina. Myocardial infarction included adjudicated fatal and nonfatal myocardial infarction plus sudden death. As shown in Figure 2, the results for the 3 endpoints (MACE, MI, and Total Mortality) were not statistically significantly different between AVANDIA and comparators.
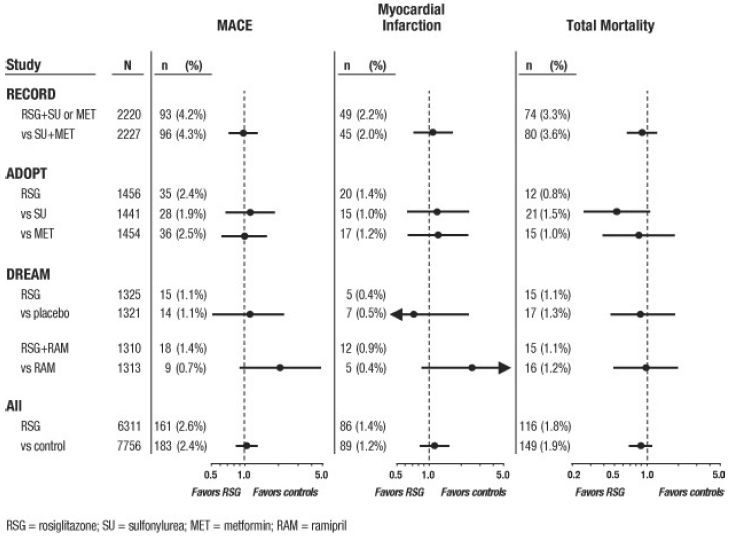
In preliminary analyses of the DREAM trial, the incidence of cardiovascular events was higher among subjects who received AVANDIA in combination with ramipril than among subjects who received ramipril alone, as illustrated in Figure 2. This finding was not confirmed in ADOPT and RECORD (active-controlled trials in patients with diabetes) in which 30% and 40% of patients respectively, reported ACE-inhibitor use at baseline.
In their entirety, the available data on the risk of myocardial ischemia are inconclusive. Definitive conclusions regarding this risk await completion of an adequately-designed cardiovascular outcome study.
There have been no clinical studies establishing conclusive evidence of macrovascular risk reduction with AVANDIA or any other oral antidiabetic drug.
Congestive Heart Failure and Myocardial Ischemia During Coadministration of AVANDIA With Insulin
In studies in which AVANDIA was added to insulin, AVANDIA increased the risk of congestive heart failure and myocardial ischemia. (See Table 2.)
Coadministration of AVANDIA and insulin is not recommended. [See Indications and Usage and WARNINGS AND PRECAUTIONS.]
In five, 26-week, controlled, randomized, double-blind trials which were included in the meta-analysis[see WARNINGS AND PRECAUTIONS] , patients with type 2 diabetes mellitus were randomized to coadministration of AVANDIA and insulin (N = 867) or insulin (N = 663). In these 5 trials, AVANDIA was added to insulin. These trials included patients with long-standing diabetes (median duration of 12 years) and a high prevalence of pre-existing medical conditions, including peripheral neuropathy, retinopathy, ischemic heart disease, vascular disease, and congestive heart failure. The total number of patients with emergent congestive heart failure was 21 (2.4%) and 7 (1.1%) in the AVANDIA plus insulin and insulin groups, respectively. The total number of patients with emergent myocardial ischemia was 24 (2.8%) and 9 (1.4%) in the AVANDIA plus insulin and insulin groups, respectively (OR 2.1 [95% CI 0.9, 5.1]). Although the event rate for congestive heart failure and myocardial ischemia was low in the studied population, consistently the event rate was 2-fold or higher with coadministration of AVANDIA and insulin. These cardiovascular events were noted at both the 4 mg and 8 mg daily doses of AVANDIA. (See Table 2.)
Table 2. Occurrence of Cardiovascular Events in 5 Controlled Trials of Addition of AVANDIA to Established Insulin Treatment
| Event* | AVANDIA + Insulin (n = 867) n (%) | Insulin (n = 663) n (%) |
| Congestive heart failure | 21 (2.4%) | 7 (1.1%) |
| Myocardial ischemia | 24 (2.8%) | 9 (1.4%) |
| Composite of cardiovascular death, myocardial infarction, or stroke | 10 (1.2%) | 5 (0.8%) |
| Stroke | 5 (0.6%) | 4 (0.6%) |
| Myocardial infarction | 4 (0.5%) | 1 (0.2%) |
| Cardiovascular death | 4 (0.5%) | 1 (0.2%) |
| All deaths | 6 (0.7%) | 1 (0.2%) |
| * Events are not exclusive; i.e., a patient with a cardiovascular death due to a myocardial infarction would be counted in 4 event categories (myocardial ischemia; cardiovascular death, myocardial infarction or stroke; myocardial infarction; cardiovascular death). | ||
In a sixth, 24-week, controlled, randomized, double-blind trial of AVANDIA and insulin coadministration, insulin was added to AVANDAMET® (rosiglitazone maleate and metformin HCl) (n = 161) and compared to insulin plus placebo (n = 158), after a single-blind 8-week run-in with AVANDAMET. Patients with edema requiring pharmacologic therapy and those with congestive heart failure were excluded at baseline and during the run-in period.
In the group receiving AVANDAMET plus insulin, there was one myocardial ischemic event and one sudden death. No myocardial ischemia was observed in the insulin group, and no congestive heart failure was reported in either treatment group.
Edema
AVANDIA should be used with caution in patients with edema. In a clinical study in healthy volunteers who received 8 mg of AVANDIA once daily for 8 weeks, there was a statistically significant increase in median plasma volume compared to placebo.
Since thiazolidinediones, including rosiglitazone, can cause fluid retention, which can exacerbate or lead to congestive heart failure, AVANDIA should be used with caution in patients at risk for heart failure. Patients should be monitored for signs and symptoms of heart failure [see BOXED WARNING, WARNINGS AND PRECAUTIONS ].
In controlled clinical trials of patients with type 2 diabetes, mild to moderate edema was reported in patients treated with AVANDIA, and may be dose related. Patients with ongoing edema were more likely to have adverse events associated with edema if started on combination therapy with insulin and AVANDIA [see ADVERSE REACTIONS].
Weight Gain
Dose-related weight gain was seen with AVANDIA alone and in combination with other hypoglycemic agents (Table 3). The mechanism of weight gain is unclear but probably involves a combination of fluid retention and fat accumulation.
In postmarketing experience, there have been reports of unusually rapid increases in weight and increases in excess of that generally observed in clinical trials. Patients who experience such increases should be assessed for fluid accumulation and volume-related events such as excessive edema and congestive heart failure [see BOXED WARNING].
Table 3. Weight Changes (kg) From Baseline at Endpoint During Clinical Trials
| Monotherapy | Duration | Control Group | AVANDIA 4 mg Median (25th, 75th percentile) | AVANDIA 8 mg Median (25th, 75th percentile) | |
| Median (25th, 75th percentile) | |||||
| 26 weeks | placebo | -0.9 (-2.8, 0.9) n = 210 | 1.0 (-0.9, 3.6) n = 436 | 3.1 (1.1, 5.8) n = 439 | |
| 52 weeks | sulfonylurea | 2.0 (0, 4.0) n = 173 | 2.0 (-0.6, 4.0) n = 150 | 2.6 (0, 5.3) n = 157 | |
| Combination therapy | |||||
| Sulfonylurea | 24-26 weeks | sulfonylurea | 0 (-1.0, 1.3) n = 1,155 | 2.2 (0.5, 4.0) n = 613 | 3.5 (1.4, 5.9) n = 841 |
| Metformin | 26 weeks | metformin | -1.4 (-3.2, 0.2) n = 175 | 0.8 (-1.0, 2.6) n = 100 | 2.1 (0, 4.3) n = 184 |
| Insulin | 26 weeks | insulin | 0.9 (-0.5, 2.7) n = 162 | 4.1 (1.4, 6.3) n = 164 | 5.4 (3.4, 7.3) n = 150 |
| Sulfonylurea + metformin | 26 weeks | sulfonylurea + metformin | 0.2 (-1.2, 1.6) n = 272 | 2.5 (0.8, 4.6) n = 275 | 4.5 (2.4, 7.3) n = 276 |
In a 4- to 6-year, monotherapy, comparative trial (ADOPT) in patients recently diagnosed with type 2 diabetes not previously treated with antidiabetic medication [see Clinical Studies], the median weight change (25th, 75th percentiles) from baseline at 4 years was 3.5 kg (0.0, 8.1) for AVANDIA, 2.0 kg (-1.0, 4.8) for glyburide, and -2.4 kg (-5.4, 0.5) for metformin.
In a 24-week study in pediatric patients aged 10 to 17 years treated with AVANDIA 4 to 8 mg daily, a median weight gain of 2.8 kg (25th, 75th percentiles: 0.0, 5.8) was reported.
Hepatic Effects
Liver enzymes should be measured prior to the initiation of therapy with AVANDIA in all patients and periodically thereafter per the clinical judgment of the healthcare professional. Therapy with AVANDIA should not be initiated in patients with increased baseline liver enzyme levels (ALT > 2.5X upper limit of normal). Patients with mildly elevated liver enzymes (ALT levels ≤ 2.5X upper limit of normal) at baseline or during therapy with AVANDIA should be evaluated to determine the cause of the liver enzyme elevation. Initiation of, or continuation of, therapy with AVANDIA in patients with mild liver enzyme elevations should proceed with caution and include close clinical follow-up, including liver enzyme monitoring, to determine if the liver enzyme elevations resolve or worsen. If at any time ALT levels increase to > 3X the upper limit of normal in patients on therapy with AVANDIA, liver enzyme levels should be rechecked as soon as possible. If ALT levels remain > 3X the upper limit of normal, therapy with AVANDIA should be discontinued.
If any patient develops symptoms suggesting hepatic dysfunction, which may include unexplained nausea, vomiting, abdominal pain, fatigue, anorexia and/or dark urine, liver enzymes should be checked. The decision whether to continue the patient on therapy with AVANDIA should be guided by clinical judgment pending laboratory evaluations. If jaundice is observed, drug therapy should be discontinued. [See ADVERSE REACTIONS.]
Macular Edema
Macular edema has been reported in postmarketing experience in some diabetic patients who were taking AVANDIA or another thiazolidinedione. Some patients presented with blurred vision or decreased visual acuity, but some patients appear to have been diagnosed on routine ophthalmologic examination. Most patients had peripheral edema at the time macular edema was diagnosed. Some patients had improvement in their macular edema after discontinuation of their thiazolidinedione. Patients with diabetes should have regular eye exams by an ophthalmologist, per the Standards of Care of the American Diabetes Association. Additionally, any diabetic who reports any kind of visual symptom should be promptly referred to an ophthalmologist, regardless of the patient's underlying medications or other physical findings. [See ADVERSE REACTIONS.]
Fractures
In a 4- to 6-year comparative study (ADOPT) of glycemic control with monotherapy in drug-naïve patients recently diagnosed with type 2 diabetes mellitus, an increased incidence of bone fracture was noted in female patients taking AVANDIA. Over the 4- to 6-year period, the incidence of bone fracture in females was 9.3% (60/645) for AVANDIA versus 3.5% (21/605) for glyburide and 5.1% (30/590) for metformin. This increased incidence was noted after the first year of treatment and persisted during the course of the study. The majority of the fractures in the women who received AVANDIA occurred in the upper arm, hand, and foot. These sites of fracture are different from those usually associated with postmenopausal osteoporosis (e.g., hip or spine). No increase in fracture rates was observed in men treated with AVANDIA. The risk of fracture should be considered in the care of patients, especially female patients, treated with AVANDIA, and attention given to assessing and maintaining bone health according to current standards of care.
Hematologic Effects
Decreases in mean hemoglobin and hematocrit occurred in a dose-related fashion in adult patients treated with AVANDIA [see ADVERSE REACTIONS]. The observed changes may be related to the increased plasma volume observed with treatment with AVANDIA.
Diabetes and Blood Glucose Control
Patients receiving AVANDIA in combination with other hypoglycemic agents may be at risk for hypoglycemia, and a reduction in the dose of the concomitant agent may be necessary.
Periodic fasting blood glucose and HbA1c measurements should be performed to monitor therapeutic response.
Ovulation
Therapy with AVANDIA, like other thiazolidinediones, may result in ovulation in some premenopausal anovulatory women. As a result, these patients may be at an increased risk for pregnancy while taking AVANDIA [see Use in Specific Populations]. Thus, adequate contraception in premenopausal women should be recommended. This possible effect has not been specifically investigated in clinical studies; therefore, the frequency of this occurrence is not known.
Although hormonal imbalance has been seen in preclinical studies [see Nonclinical Toxicology], the clinical significance of this finding is not known. If unexpected menstrual dysfunction occurs, the benefits of continued therapy with AVANDIA should be reviewed.
Adverse Reactions
Clinical Trial Experience
Adult
In clinical trials, approximately 9,900 patients with type 2 diabetes have been treated with AVANDIA.
Short-Term Trials of AVANDIA as Monotherapy and in Combination With Other Hypoglycemic Agents
The incidence and types of adverse events reported in short-term clinical trials of AVANDIA as monotherapy are shown in Table 4.
Table 4. Adverse Events ( ≥ 5% in Any Treatment Group) Reported by Patients in Short-Term*Double-Blind Clinical Trials With AVANDIA as Monotherapy
| Preferred Term | AVANDIA Monotherapy N = 2,526 % | Placebo N = 601 % | Metformin N = 225 % | Sulfonylureas†N = 626 % |
| Upper respiratory tract infection | 9.9 | 8.7 | 8.9 | 7.3 |
| Injury | 7.6 | 4.3 | 7.6 | 6.1 |
| Headache | 5.9 | 5.0 | 8.9 | 5.4 |
| Back pain | 4.0 | 3.8 | 4.0 | 5.0 |
| Hyperglycemia | 3.9 | 5.7 | 4.4 | 8.1 |
| Fatigue | 3.6 | 5.0 | 4.0 | 1.9 |
| Sinusitis | 3.2 | 4.5 | 5.3 | 3.0 |
| Diarrhea | 2.3 | 3.3 | 15.6 | 3.0 |
| Hypoglycemia | 0.6 | 0.2 | 1.3 | 5.9 |
| * Short-term trials ranged from 8 weeks to 1 year. †Includes patients receiving glyburide (N = 514), gliclazide (N = 91), or glipizide (N = 21). | ||||
Overall, the types of adverse reactions without regard to causality reported when AVANDIA was used in combination with a sulfonylurea or metformin were similar to those during monotherapy with AVANDIA.
Events of anemia and edema tended to be reported more frequently at higher doses, and were generally mild to moderate in severity and usually did not require discontinuation of treatment with AVANDIA.
In double-blind studies, anemia was reported in 1.9% of patients receiving AVANDIA as monotherapy compared to 0.7% on placebo, 0.6% on sulfonylureas, and 2.2% on metformin. Reports of anemia were greater in patients treated with a combination of AVANDIA and metformin (7.1%) and with a combination of AVANDIA and a sulfonylurea plus metformin (6.7%) compared to monotherapy with AVANDIA or in combination with a sulfonylurea (2.3%). Lower pre-treatment hemoglobin/hematocrit levels in patients enrolled in the metformin combination clinical trials may have contributed to the higher reporting rate of anemia in these studies [see ADVERSE REACTIONS].
In clinical trials, edema was reported in 4.8% of patients receiving AVANDIA as monotherapy compared to 1.3% on placebo, 1.0% on sulfonylureas, and 2.2% on metformin. The reporting rate of edema was higher for AVANDIA 8 mg in sulfonylurea combinations (12.4%) compared to other combinations, with the exception of insulin. Edema was reported in 14.7% of patients receiving AVANDIA in the insulin combination trials compared to 5.4% on insulin alone. Reports of new onset or exacerbation of congestive heart failure occurred at rates of 1% for insulin alone, and 2% (4 mg) and 3% (8 mg) for insulin in combination with AVANDIA [see BOXED WARNING and WARNINGS AND PRECAUTIONS].
In controlled combination therapy studies with sulfonylureas, mild to moderate hypoglycemic symptoms, which appear to be dose related, were reported. Few patients were withdrawn for hypoglycemia ( < 1%) and few episodes of hypoglycemia were considered to be severe ( < 1%). Hypoglycemia was the most frequently reported adverse event in the fixed-dose insulin combination trials, although few patients withdrew for hypoglycemia (4 of 408 for AVANDIA plus insulin and 1 of 203 for insulin alone). Rates of hypoglycemia, confirmed by capillary blood glucose concentration ≤ 50 mg/dL, were 6% for insulin alone and 12% (4 mg) and 14% (8 mg) for insulin in combination with AVANDIA. [See WARNINGS AND PRECAUTIONS.]
Long-Term Trial of AVANDIA as Monotherapy
A 4- to 6-year study (ADOPT) compared the use of AVANDIA (n = 1,456), glyburide (n = 1,441), and metformin (n = 1,454) as monotherapy in patients recently diagnosed with type 2 diabetes who were not previously treated with antidiabetic medication. Table 5 presents adverse reactions without regard to causality; rates are expressed per 100 patient-years (PY) exposure to account for the differences in exposure to study medication across the 3 treatment groups.
In ADOPT, fractures were reported in a greater number of women treated with AVANDIA (9.3%, 2.7/100 patient-years) compared to glyburide (3.5%, 1.3/100 patient-years) or metformin (5.1%, 1.5/100 patient-years).
The majority of the fractures in the women who received rosiglitazone were reported in the upper arm, hand, and foot. [See WARNINGS AND PRECAUTIONS.] The observed incidence of fractures for male patients was similar among the 3 treatment groups.
Table 5. On-Therapy Adverse Events ( ≥ 5 Events/100 Patient-Years [PY]) in Any Treatment Group Reported in a 4- to 6-Year Clinical Trial of AVANDIA as Monotherapy (ADOPT)
| AVANDIA N = 1,456 PY = 4,954 | Glyburide N = 1,441 PY = 4,244 | Metformin N = 1,454 PY = 4,906 | |
| Nasopharyngitis | 6.3 | 6.9 | 6.6 |
| Back pain | 5.1 | 4.9 | 5.3 |
| Arthralgia | 5.0 | 4.8 | 4.2 |
| Hypertension | 4.4 | 6.0 | 6.1 |
| Upper respiratory tract infection | 4.3 | 5.0 | 4.7 |
| Hypoglycemia | 2.9 | 13.0 | 3.4 |
| Diarrhea | 2.5 | 3.2 | 6.8 |
Pediatric
Avandia has been evaluated for safety in a single, active-controlled trial of pediatric patients with type 2 diabetes in which 99 were treated with Avandia and 101 were treated with metformin. The most common adverse reactions (>10%) without regard to causality for either Avandia or metformin were headache (17% versus 14%), nausea (4% versus 11%), nasopharyngitis (3% versus 12%), and diarrhea (1% versus 13%). In this study, one case of diabetic ketoacidosis was reported in the metformin group. In addition, there were 3 patients in the rosiglitazone group who had FPG of ∼300 mg/dL, 2+ ketonuria, and an elevated anion gap.
Laboratory Abnormalities
Hematologic
Decreases in mean hemoglobin and hematocrit occurred in a dose-related fashion in adult patients treated with Avandia (mean decreases in individual studies as much as 1.0 g/dL hemoglobin and as much as 3.3% hematocrit). The changes occurred primarily during the first 3 months following initiation of therapy with Avandia or following a dose increase in Avandia. The time course and magnitude of decreases were similar in patients treated with a combination of Avandia and other hypoglycemic agents or monotherapy with Avandia. Pre-treatment levels of hemoglobin and hematocrit were lower in patients in metformin combination studies and may have contributed to the higher reporting rate of anemia. In a single study in pediatric patients, decreases in hemoglobin and hematocrit (mean decreases of 0.29 g/dL and 0.95%, respectively) were reported. Small decreases in hemoglobin and hematocrit have also been reported in pediatric patients treated with Avandia. White blood cell counts also decreased slightly in adult patients treated with Avandia. Decreases in hematologic parameters may be related to increased plasma volume observed with treatment with Avandia.
Lipids
Changes in serum lipids have been observed following treatment with Avandia in adults [see Clinical Pharmacology ]. Small changes in serum lipid parameters were reported in children treated with Avandia for 24 weeks.
Serum Transaminase Levels
In pre-approval clinical studies in 4,598 patients treated with Avandia (3,600 patient-years of exposure) and in a long-term 4- to 6-year study in 1,456 patients treated with Avandia (4,954 patient-years exposure), there was no evidence of drug-induced hepatotoxicity.
In pre-approval controlled trials, 0.2% of patients treated with Avandia had elevations in ALT >3X the upper limit of normal compared to 0.2% on placebo and 0.5% on active comparators. The ALT elevations in patients treated with Avandia were reversible. Hyperbilirubinemia was found in 0.3% of patients treated with Avandia compared with 0.9% treated with placebo and 1% in patients treated with active comparators. In pre-approval clinical trials, there were no cases of idiosyncratic drug reactions leading to hepatic failure. [See Warnings and Precautions]
In the 4- to 6-year ADOPT trial, patients treated with Avandia (4,954 patient-years exposure), glyburide (4,244 patient-years exposure), or metformin (4,906 patient-years exposure), as monotherapy, had the same rate of ALT increase to >3X upper limit of normal (0.3 per 100 patient-years exposure).
Postmarketing Experience
In addition to adverse reactions reported from clinical trials, the events described below have been identified during post-approval use of Avandia. Because these events are reported voluntarily from a population of unknown size, it is not possible to reliably estimate their frequency or to always establish a causal relationship to drug exposure.
In patients receiving thiazolidinedione therapy, serious adverse events with or without a fatal outcome, potentially related to volume expansion (e.g., congestive heart failure, pulmonary edema, and pleural effusions) have been reported [see Boxed Warning and Warnings and Precautions].
There are postmarketing reports with Avandia of hepatitis, hepatic enzyme elevations to 3 or more times the upper limit of normal, and hepatic failure with and without fatal outcome, although causality has not been established.
Rash, pruritus, urticaria, angioedema, anaphylactic reaction, and Stevens-Johnson syndrome have been reported rarely.
Reports of new onset or worsening diabetic macular edema with decreased visual acuity have also been received [see Warnings and Precautions].
Drug Interactions
CYP2C8 Inhibitors and Inducers
An inhibitor of CYP2C8 (e.g., gemfibrozil) may increase the AUC of rosiglitazone and an inducer of CYP2C8 (e.g., rifampin) may decrease the AUC of rosiglitazone. Therefore, if an inhibitor or an inducer of CYP2C8 is started or stopped during treatment with rosiglitazone, changes in diabetes treatment may be needed based upon clinical response. [See CLINICAL PHARMACOLOGY.]
Use in Specific Populations
Pregnancy
Pregnancy Category C.
All pregnancies have a background risk of birth defects, loss, or other adverse outcome regardless of drug exposure. This background risk is increased in pregnancies complicated by hyperglycemia and may be decreased with good metabolic control. It is essential for patients with diabetes or history of gestational diabetes to maintain good metabolic control before conception and throughout pregnancy. Careful monitoring of glucose control is essential in such patients. Most experts recommend that insulin monotherapy be used during pregnancy to maintain blood glucose levels as close to normal as possible.
Human Data: Rosiglitazone has been reported to cross the human placenta and bedetectable in fetal tissue. The clinical significance of these findings is unknown. There are no adequate and well-controlled studies in pregnant women. AVANDIA should not be used during pregnancy.
Animal Studies: There was no effect on implantation or the embryo with rosiglitazone treatment during early pregnancy in rats, but treatment during mid-late gestation was associated with fetal death and growth retardation in both rats and rabbits. Teratogenicity was not observed at doses up to 3 mg/kg in rats and 100 mg/kg in rabbits (approximately 20 and 75 times human AUC at the maximum recommended human daily dose, respectively). Rosiglitazone caused placental pathology in rats (3 mg/kg/day). Treatment of rats during gestation through lactation reduced litter size, neonatal viability, and postnatal growth, with growth retardation reversible after puberty. For effects on the placenta, embryo/fetus, and offspring, the no-effect dose was 0.2 mg/kg/day in rats and 15 mg/kg/day in rabbits. These no-effect levels are approximately 4 times human AUC at the maximum recommended human daily dose. Rosiglitazone reduced the number of uterine implantations and live offspring when juvenile female rats were treated at 40 mg/kg/day from 27 days of age through to sexual maturity (approximately 68 times human AUC at the maximum recommended daily dose). The no-effect level was 2 mg/kg/day (approximately 4 times human AUC at the maximum recommended daily dose). There was no effect on pre- or post-natal survival or growth.
Labor and Delivery
The effect of rosiglitazone on labor and delivery in humans is not known.
Nursing Mothers
Drug-related material was detected in milk from lactating rats. It is not known whether AVANDIA is excreted in human milk. Because many drugs are excreted in human milk, AVANDIA should not be administered to a nursing woman.
Pediatric Use
After placebo run-in including diet counseling, children with type 2 diabetes mellitus, aged 10 to 17 years and with a baseline mean body mass index (BMI) of 33 kg/m , were randomized to treatment with 2 mg twice daily of AVANDIA (n = 99) or 500 mg twice daily of metformin (n = 101) in a 24-week, double-blind clinical trial. As expected, FPG decreased in patients naïve to diabetes medication (n = 104) and increased in patients withdrawn from prior medication (usually metformin) (n = 90) during the run-in period. After at least 8 weeks of treatment, 49% of patients treated with AVANDIA and 55% of metformin-treated patients had their dose doubled if FPG >126 mg/dL. For the overall intent-to-treat population, at week 24, the mean change from baseline in HbA1c was -0.14% with AVANDIA and -0.49% with metformin. There was an insufficient number of patients in this study to establish statistically whether these
observed mean treatment effects were similar or different. Treatment effects differed for patients naïve to therapy with antidiabetic drugs and for patients previously treated with antidiabetic therapy (Table 6).
Table 6. Week 24 FPG and HbA1c Change From Baseline Last-Observation-Carried Forward in Children With Baseline HbA1c > 6.5%
| Naïve Patients | Previously-Treated Patients | |||
Metformin N = 40 | Rosiglitazone N = 45 | Metformin N = 43 | Rosiglitazone N = 32 | |
| FPG (mg/dL) | ||||
| Baseline (mean) | 170 | 165 | 221 | 205 |
| Change from baseline (mean) | -21 | -11 | -33 | -5 |
| Adjusted treatment difference* (rosiglitazone-metformin)†(95% CI) | 8 (-15, 30) | 21 (-9, 51) | ||
| % of patients with ≥ 30 mg/dL decrease from baseline | 43% | 27% | 44% | 28% |
| HbA1c (%) | ||||
| Baseline (mean) | 8.3 | 8.2 | 8.8 | 8.5 |
| Change from baseline (mean) | -0.7 | -0.5 | -0.4 | 0.1 |
| Adjusted treatment difference* (rosiglitazone-metformin)†(95% CI) | 0.2 (-0.6, 0.9) | 0.5 (-0.2, 1.3) | ||
| % of patients with ≥ 0.7% decrease from baseline | 63% | 52% | 54% | 31% |
| * Change from baseline means are least squares means adjusting for baseline HbA1c, gender, and region. †Positive values for the difference favor metformin. | ||||
Treatment differences depended on baseline BMI or weight such that the effects of AVANDIA and metformin appeared more closely comparable among heavier patients. The median weight gain was 2.8 kg with rosiglitazone and 0.2 kg with metformin [see WARNINGS AND PRECAUTIONS]. Fifty-four percent of patients treated with rosiglitazone and 32% of patients treated with metformin gained ≥ 2 kg, and 33% of patients treated with rosiglitazone and 7% of patients treated with metformin gained ≥ 5 kg on study.
Adverse events observed in this study are described in Adverse Reactions).
Figure 3. Mean HbA1c Over Time in a 24-Week Study of AVANDIA and Metformin in Pediatric Patients — Drug-Naïve Subgroup
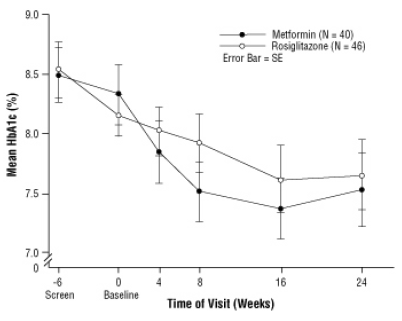
Geriatric Use
Results of the population pharmacokinetic analysis showed that age does not significantly affect the pharmacokinetics of rosiglitazone [see CLINICAL PHARMACOLOGY]. Therefore, no dosage adjustments are required for the elderly. In controlled clinical trials, no overall differences in safety and effectiveness between older ( ≥ 65 years) and younger ( < 65 years) patients were observed.
Overdosage
Limited data are available with regard to overdosage in humans. In clinical studies in volunteers, AVANDIA has been administered at single oral doses of up to 20 mg and was well-tolerated. In the event of an overdose, appropriate supportive treatment should be initiated as dictated by the patient's clinical status.
Description
AVANDIA (rosiglitazone maleate) is an oral antidiabetic agent which acts primarily by increasing insulin sensitivity. AVANDIA improves glycemic control while reducing circulating insulin levels.
Rosiglitazone maleate is not chemically or functionally related to the sulfonylureas, the biguanides, or the alpha-glucosidase inhibitors.
Chemically, rosiglitazone maleate is ( ±)-5-[[4-[2-(methyl-2-pyridinylamino)ethoxy]phenyl]methyl]-2,4-thiazolidinedione, (Z)-2-butenedioate (1:1) with a molecular weight of 473.52 (357.44 free base). The molecule has a single chiral center and is present as a racemate. Due to rapid interconversion, the enantiomers are functionally indistinguishable. The structural formula of rosiglitazone maleate is:
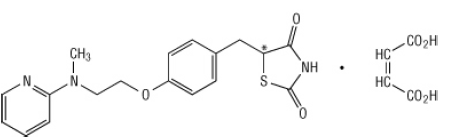
The molecular formula is C18H19N3O3S-C4H4O4. Rosiglitazone maleate is a white to off-white solid with a melting point range of 122 to 123°C. The pKa values of rosiglitazone maleate are 6.8 and 6.1. It is readily soluble in ethanol and a buffered aqueous solution with pH of 2.3; solubility decreases with increasing pH in the physiological range.
Each pentagonal film-coated TILTAB tablet contains rosiglitazone maleate equivalent to rosiglitazone, 2 mg, 4 mg, or 8 mg, for oral administration. Inactive ingredients are: Hypromellose 2910, lactose monohydrate, magnesium stearate, microcrystalline cellulose, polyethylene glycol 3000, sodium starch glycolate, titanium dioxide, triacetin, and 1 or more of the following: Synthetic red and yellow iron oxides and talc.
Clinical Pharmacology
Mechanism of Action
Rosiglitazone, a member of the thiazolidinedione class of antidiabetic agents, improves glycemic control by improving insulin sensitivity. Rosiglitazone is a highly selective and potent agonist for the peroxisome proliferator-activated receptor-gamma (PPARγ). In humans, PPAR receptors are found in key target tissues for insulin action such as adipose tissue, skeletal muscle, and liver. Activation of PPARγ nuclear receptors regulates the transcription of insulin-responsive genes involved in the control of glucose production, transport, and utilization. In addition, PPARγ-responsive genes also participate in the regulation of fatty acid metabolism.
Insulin resistance is a common feature characterizing the pathogenesis of type 2 diabetes. The antidiabetic activity of rosiglitazone has been demonstrated in animal models of type 2 diabetes in which hyperglycemia and/or impaired glucose tolerance is a consequence of insulin resistance in target tissues. Rosiglitazone reduces blood glucose concentrations and reduces hyperinsulinemia in the ob/ob obese mouse, db/db diabetic mouse, and fa/fa fatty Zucker rat.
In animal models, the antidiabetic activity of rosiglitazone was shown to be mediated by increased sensitivity to insulin's action in the liver, muscle, and adipose tissues. Pharmacological studies in animal models indicate that rosiglitazone inhibits hepatic gluconeogenesis. The expression of the insulin-regulated glucose transporter GLUT-4 was increased in adipose tissue. Rosiglitazone did not induce hypoglycemia in animal models of type 2 diabetes and/or impaired glucose tolerance.
Pharmacodynamics
Patients with lipid abnormalities were not excluded from clinical trials of AVANDIA.
In all 26-week controlled trials, across the recommended dose range, AVANDIA as monotherapy was associated with increases in total cholesterol, LDL, and HDL and decreases in free fatty acids. These changes were statistically significantly different from placebo or glyburide controls (Table 7).
Increases in LDL occurred primarily during the first 1 to 2 months of therapy with AVANDIA and LDL levels remained elevated above baseline throughout the trials. In contrast, HDL continued to rise over time. As a result, the LDL/HDL ratio peaked after 2 months of therapy and then appeared to decrease over time. Because of the temporal nature of lipid changes, the 52-week glyburide-controlled study is most pertinent to assess long-term effects on lipids. At baseline, week 26, and week 52, mean LDL/HDL ratios were 3.1, 3.2, and 3.0, respectively, for AVANDIA 4 mg twice daily. The corresponding values for glyburide were 3.2, 3.1, and 2.9. The differences in change from baseline between AVANDIA and glyburide at week 52 were statistically significant.
The pattern of LDL and HDL changes following therapy with AVANDIA in combination with other hypoglycemic agents were generally similar to those seen with AVANDIA in monotherapy.
The changes in triglycerides during therapy with AVANDIA were variable and were generally not statistically different from placebo or glyburide controls.
Table 7. Summary of Mean Lipid Changes in 26-Week Placebo-Controlled and 52-Week Glyburide-Controlled Monotherapy Studies
| Placebo-Controlled Studies Week 26 | Glyburide-Controlled Study Week 26 and Week 52 | ||||||
| Placebo | AVANDIA | Glyburide Titration | AVANDIA 8 mg | ||||
| 4 mg daily* | 8 mg daily* | Wk 26 | Wk 52 | Wk 26 | Wk 52 | ||
| Free fatty acids | |||||||
| N | 207 | 428 | 436 | 181 | 168 | 166 | 145 |
| Baseline (mean) % | 18.1 | 17.5 | 17.9 | 26.4 | 26.4 | 26.9 | 26.6 |
| Change from baseline (mean) | +0.2% | -7.8% | -14.7% | -2.4% | -4.7% | -20.8% | -21.5% |
| LDL | |||||||
| N | 190 | 400 | 374 | 175 | 160 | 161 | 133 |
| Baseline (mean) % | 123.7 | 126.8 | 125.3 | 142.7 | 141.9 | 142.1 | 142.1 |
| Change from baseline (mean) | +4.8% | +14.1% | +18.6% | -0.9% | -0.5% | +11.9% | +12.1% |
| HDL | |||||||
| N | 208 | 429 | 436 | 184 | 170 | 170 | 145 |
| Baseline (mean) % | 44.1 | 44.4 | 43.0 | 47.2 | 47.7 | 48.4 | 48.3 |
| Change from baseline (mean) | +8.0% | +11.4% | +14.2% | +4.3% | +8.7% | +14.0% | +18.5% |
| * Once daily and twice daily dosing groups were combined. | |||||||
Pharmacokinetics
Maximum plasma concentration (Cmax) and the area under the curve (AUC) of rosiglitazone increase in a dose-proportional manner over the therapeutic dose range (Table 8). The elimination half-life is 3 to 4 hours and is independent of dose.
Table 8. Mean (SD) Pharmacokinetic Parameters for Rosiglitazone Following Single Oral Doses (N = 32)
| Parameter | 1 mg Fasting | 2 mg Fasting | 8 mg Fasting | 8 mg Fed |
| AUC0-inf [ng-hr/mL] | 358 (112) | 733 (184) | 2,971 (730) | 2,890 (795) |
| Cmax [ng/mL] | 76 (13) | 156 (42) | 598 (117) | 432 (92) |
| Half-life [hr] | 3.16 (0.72) | 3.15 (0.39) | 3.37 (0.63) | 3.59 (0.70) |
| CL/F* [L/hr] | 3.03 (0.87) | 2.89 (0.71) | 2.85 (0.69) | 2.97 (0.81) |
| * CL/F = Oral clearance. | ||||
Absorption
The absolute bioavailability of rosiglitazone is 99%. Peak plasma concentrations are observed about 1 hour after dosing. Administration of rosiglitazone with food resulted in no change in overall exposure (AUC), but there was an approximately 28% decrease in Cmax and a delay in Tmax (1.75 hours). These changes are not likely to be clinically significant; therefore, AVANDIA may be administered with or without food.
Distribution
The mean (CV%) oral volume of distribution (Vss/F) of rosiglitazone is approximately 17.6 (30%) liters, based on a population pharmacokinetic analysis. Rosiglitazone is approximately 99.8% bound to plasma proteins, primarily albumin.
Metabolism
Rosiglitazone is extensively metabolized with no unchanged drug excreted in the urine. The major routes of metabolism were N-demethylation and hydroxylation, followed by conjugation with sulfate and glucuronic acid. All the circulating metabolites are considerably less potent than parent and, therefore, are not expected to contribute to the insulin-sensitizing activity of rosiglitazone.
In vitro data demonstrate that rosiglitazone is predominantly metabolized by Cytochrome P450 (CYP) isoenzyme 2C8, with CYP2C9 contributing as a minor pathway.
Excretion
Following oral or intravenous administration of [14C]rosiglitazone maleate, approximately 64% and 23% of the dose was eliminated in the urine and in the feces, respectively. The plasma half-life of [14C]related material ranged from 103 to 158 hours.
Population Pharmacokinetics in Patients With Type 2 Diabetes
Population pharmacokinetic analyses from 3 large clinical trials including 642 men and 405 women with type 2 diabetes (aged 35 to 80 years) showed that the pharmacokinetics of rosiglitazone are not influenced by age, race, smoking, or alcohol consumption. Both oral clearance (CL/F) and oral steady-state volume of distribution (Vss/F) were shown to increase with increases in body weight. Over the weight range observed in these analyses (50 to 150 kg), the range of predicted CL/F and Vss/F values varied by < 1.7-fold and < 2.3-fold, respectively.
Additionally, rosiglitazone CL/F was shown to be influenced by both weight and gender, being lower (about 15%) in female patients.
Special Populations
Geriatric
Results of the population pharmacokinetic analysis (n = 716 < 65 years; n = 331 ≥ 65 years) showed that age does not significantly affect the pharmacokinetics of rosiglitazone.
Gender
Results of the population pharmacokinetics analysis showed that the mean oral clearance of rosiglitazone in female patients (n = 405) was approximately 6% lower compared to male patients of the same body weight (n = 642).
As monotherapy and in combination with metformin, AVANDIA improved glycemic control in both males and females. In metformin combination studies, efficacy was demonstrated with no gender differences in glycemic response.
In monotherapy studies, a greater therapeutic response was observed in females; however, in more obese patients, gender differences were less evident. For a given body mass index (BMI), females tend to have a greater fat mass than males. Since the molecular target PPARγ is expressed in adipose tissues, this differentiating characteristic may account, at least in part, for the greater response to AVANDIA in females. Since therapy should be individualized, no dose adjustments are necessary based on gender alone.
Hepatic Impairment
Unbound oral clearance of rosiglitazone was significantly lower in patients with moderate to severe liver disease (Child-Pugh Class B/C) compared to healthy subjects. As a result, unbound Cmax and AUC0-inf were increased 2- and 3-fold, respectively. Elimination half-life for rosiglitazone was about 2 hours longer in patients with liver disease, compared to healthy subjects.
Therapy with AVANDIA should not be initiated if the patient exhibits clinical evidence of active liver disease or increased serum transaminase levels (ALT > 2.5X upper limit of normal) at baseline [see WARNINGS AND PRECAUTIONS].
Pediatric
Pharmacokinetic parameters of rosiglitazone in pediatric patients were established using a population pharmacokinetic analysis with sparse data from 96 pediatric patients in a single pediatric clinical trial including 33 males and 63 females with ages ranging from 10 to 17 years (weights ranging from 35 to 178.3 kg). Population mean CL/F and V/F of rosiglitazone were 3.15 L/hr and 13.5 L, respectively. These estimates of CL/F and V/F were consistent with the typical parameter estimates from a prior adult population analysis.
Renal Impairment
There are no clinically relevant differences in the pharmacokinetics of rosiglitazone in patients with mild to severe renal impairment or in hemodialysis-dependent patients compared to subjects with normal renal function. No dosage adjustment is therefore required in such patients receiving AVANDIA. Since metformin is contraindicated in patients with renal impairment, coadministration of metformin with AVANDIA is contraindicated in these patients.
Race
Results of a population pharmacokinetic analysis including subjects of Caucasian, black, and other ethnic origins indicate that race has no influence on the pharmacokinetics of rosiglitazone.
Drug-Drug Interactions
Drugs That Inhibit, Induce, or are Metabolized by Cytochrome P450
In vitro drug metabolism studies suggest that rosiglitazone does not inhibit any of the major P450 enzymes at clinically relevant concentrations. In vitro data demonstrate that rosiglitazone is predominantly metabolized by CYP2C8, and to a lesser extent, 2C9. AVANDIA (4 mg twice daily) was shown to have no clinically relevant effect on the pharmacokinetics of nifedipine and oral contraceptives (ethinyl estradiol and norethindrone), which are predominantly metabolized by CYP3A4.
Gemfibrozil
Concomitant administration of gemfibrozil (600 mg twice daily), an inhibitor of CYP2C8, and rosiglitazone (4 mg once daily) for 7 days increased rosiglitazone AUC by 127%, compared to the administration of rosiglitazone (4 mg once daily) alone. Given the potential for dose-related adverse events with rosiglitazone, a decrease in the dose of rosiglitazone may be needed when gemfibrozil is introduced [see DRUG INTERACTIONS].
Rifampin
Rifampin administration (600 mg once a day), an inducer of CYP2C8, for 6 days is reported to decrease rosiglitazone AUC by 66%, compared to the administration of rosiglitazone (8 mg) alone [see DRUG INTERACTIONS].4
Glyburide
AVANDIA (2 mg twice daily) taken concomitantly with glyburide (3.75 to 10 mg/day) for 7 days did not alter the mean steady-state 24-hour plasma glucose concentrations in diabetic patients stabilized on glyburide therapy. Repeat doses of AVANDIA (8 mg once daily) for 8 days in healthy adult Caucasian subjects caused a decrease in glyburide AUC and Cmax of approximately 30%. In Japanese subjects, glyburide AUC and Cmax slightly increased following coadministration of AVANDIA.
Glimepiride
Single oral doses of glimepiride in 14 healthy adult subjects had no clinically significant effect on the steady-state pharmacokinetics of AVANDIA. No clinically significant reductions in glimepiride AUC and Cmax were observed after repeat doses of AVANDIA (8 mg once daily) for 8 days in healthy adult subjects.
Metformin
Concurrent administration of AVANDIA (2 mg twice daily) and metformin (500 mg twice daily) in healthy volunteers for 4 days had no effect on the steady-state pharmacokinetics of either metformin or rosiglitazone.
Acarbose
Coadministration of acarbose (100 mg three times daily) for 7 days in healthy volunteers had no clinically relevant effect on the pharmacokinetics of a single oral dose of AVANDIA.
Digoxin
Repeat oral dosing of AVANDIA (8 mg once daily) for 14 days did not alter the steady-state pharmacokinetics of digoxin (0.375 mg once daily) in healthy volunteers.
Warfarin
Repeat dosing with AVANDIA had no clinically relevant effect on the steady-state pharmacokinetics of warfarin enantiomers.
Ethanol
A single administration of a moderate amount of alcohol did not increase the risk of acute hypoglycemia in type 2 diabetes mellitus patients treated with AVANDIA.
Ranitidine
Pretreatment with ranitidine (150 mg twice daily for 4 days) did not alter the pharmacokinetics of either single oral or intravenous doses of rosiglitazone in healthy volunteers.
These results suggest that the absorption of oral rosiglitazone is not altered in conditions accompanied by increases in gastrointestinal pH.
Nonclinical Toxicology
Carcinogenesis, Mutagenesis, Impairment of Fertility
Carcinogenesis:
A 2-year carcinogenicity study was conducted in Charles River CD-1 mice at doses of 0.4, 1.5, and 6 mg/kg/day in the diet (highest dose equivalent to approximately 12 times human AUC at the maximum recommended human daily dose). Sprague-Dawley rats were dosed for 2 years by oral gavage at doses of 0.05, 0.3, and 2 mg/kg/day (highest dose equivalent to approximately 10 and 20 times human AUC at the maximum recommended human daily dose for male and female rats, respectively).
Rosiglitazone was not carcinogenic in the mouse. There was an increase in incidence of adipose hyperplasia in the mouse at doses 1.5 mg/kg/day (approximately 2 times human AUC at the maximum recommended human daily dose). In rats, there was a significant increase in the incidence of benign adipose tissue tumors (lipomas) at doses 0.3 mg/kg/day (approximately 2 times human AUC at the maximum recommended human daily dose). These proliferative changes in both species are considered due to the persistent pharmacological overstimulation of adipose tissue.
Mutagenesis:
Rosiglitazone was not mutagenic or clastogenic in the in vitro bacterial assays for gene mutation, the in vitro chromosome aberration test in human lymphocytes, the in vivo mouse micronucleus test, and the in vivo/in vitro rat UDS assay. There was a small (about 2-fold) increase in mutation in the in vitro mouse lymphoma assay in the presence of metabolic activation.
Impairment of Fertility:
Rosiglitazone had no effects on mating or fertility of male rats given up to 40 mg/kg/day (approximately 116 times human AUC at the maximum recommended human daily dose). Rosiglitazone altered estrous cyclicity (2 mg/kg/day) and reduced fertility (40 mg/kg/day) of female rats in association with lower plasma levels of progesterone and estradiol (approximately 20 and 200 times human AUC at the maximum recommended human daily dose, respectively). No such effects were noted at 0.2 mg/kg/day (approximately 3 times human AUC at the maximum recommended human daily dose). In juvenile rats dosed from 27 days of age through to sexual maturity (at up to 40 mg/kg/day), there was no effect on male reproductive performance, or on estrous cyclicity, mating performance or pregnancy incidence in females (approximately 68 times human AUC at the maximum recommended human daily dose). In monkeys, rosiglitazone (0.6 and 4.6 mg/kg/day; approximately 3 and 15 times human AUC at the maximum recommended human daily dose, respectively) diminished the follicular phase rise in serum estradiol with consequential reduction in the luteinizing hormone surge, lower luteal phase progesterone levels, and amenorrhea. The mechanism for these effects appears to be direct inhibition of ovarian steroidogenesis.
Animal Toxicology
Heart weights were increased in mice (3 mg/kg/day), rats (5 mg/kg/day), and dogs (2 mg/kg/day) with rosiglitazone treatments (approximately 5, 22, and 2 times human AUC at the maximum recommended human daily dose, respectively). Effects in juvenile rats were consistent with those seen in adults. Morphometric measurement indicated that there was hypertrophy in cardiac ventricular tissues, which may be due to increased heart work as a result of plasma volume expansion.
Clinical Studies
Monotherapy
In clinical studies, treatment with AVANDIA resulted in an improvement in glycemic control, as measured by FPG and HbA1c, with a concurrent reduction in insulin and C-peptide. Postprandial glucose and insulin were also reduced. This is consistent with the mechanism of action of AVANDIA as an insulin sensitizer.
The maximum recommended daily dose is 8 mg. Dose-ranging studies suggested that no additional benefit was obtained with a total daily dose of 12 mg.
Short-Term Clinical Studies: A total of 2,315 patients with type 2 diabetes, previously treated with diet alone or antidiabetic medication(s), were treated with AVANDIA as monotherapy in 6 double-blind studies, which included two 26-week placebo-controlled studies, one 52-week glyburide-controlled study, and 3 placebo-controlled dose-ranging studies of 8 to 12 weeks duration. Previous antidiabetic medication(s) were withdrawn and patients entered a 2 to 4 week placebo run-in period prior to randomization.
Two 26-week, double-blind, placebo-controlled trials, in patients with type 2 diabetes (n = 1,401) with inadequate glycemic control (mean baseline FPG approximately 228 mg/dL [101 to 425 mg/dL] and mean baseline HbA1c 8.9% [5.2% to 16.2%]), were conducted. Treatment with AVANDIA produced statistically significant improvements in FPG and HbA1c compared to baseline and relative to placebo. Data from one of these studies are summarized in Table 9.
Table 9: Glycemic Parameters in a 26-Week Placebo-Controlled Trial
| Placebo N = 173 | AVANDIA | AVANDIA | |||
| 4 mg once daily N = 180 | 2 mg twice daily N = 186 | 8 mg once daily N = 181 | 4 mg twice daily N = 187 | ||
| FPG (mg/dL) | |||||
| Baseline (mean) | 225 | 229 | 225 | 228 | 228 |
| Change from baseline (mean) | 8 | -25 | -35 | -42 | -55 |
| Difference from placebo (adjusted mean) | - | -31* | -43* | -49* | -62* |
| % of patients with ≥ 30 mg/dL decrease from baseline | 19% | 45% | 54% | 58% | 70% |
| HbA1c (%) | |||||
| Baseline (mean) | 8.9 | 8.9 | 8.9 | 8.9 | 9.0 |
| Change from baseline (mean) | 0.8 | 0.0 | -0.1 | -0.3 | -0.7 |
| Difference from placebo (adjusted mean) | - | -0.8* | -0.9* | -1.1* | -1.5* |
| % of patients with ≥ 0.7% decrease from baseline | 9% | 28% | 29% | 39% | 54% |
| * p < 0.0001 compared to placebo. | |||||
When administered at the same total daily dose, AVANDIA was generally more effective in reducing FPG and HbA1c when administered in divided doses twice daily compared to once daily doses. However, for HbA1c, the difference between the 4 mg once daily and 2 mg twice daily doses was not statistically significant.
Long-Term Clinical Studies
Long-term maintenance of effect was evaluated in a 52-week, double-blind, glyburide-controlled trial in patients with type 2 diabetes. Patients were randomized to treatment with AVANDIA 2 mg twice daily (N = 195) or AVANDIA 4 mg twice daily (N = 189) or glyburide (N = 202) for 52 weeks. Patients receiving glyburide were given an initial dosage of either 2.5 mg/day or 5.0 mg/day. The dosage was then titrated in 2.5 mg/day increments over the next 12 weeks, to a maximum dosage of 15.0 mg/day in order to optimize glycemic control. Thereafter, the glyburide dose was kept constant.
The median titrated dose of glyburide was 7.5 mg. All treatments resulted in a statistically significant improvement in glycemic control from baseline (Figure 4 and Figure 5). At the end of week 52, the reduction from baseline in FPG and HbA1c was -40.8 mg/dL and -0.53% with AVANDIA 4 mg twice daily; -25.4 mg/dL and -0.27% with AVANDIA 2 mg twice daily; and -30.0 mg/dL and -0.72% with glyburide. For HbA1c, the difference between AVANDIA 4 mg twice daily and glyburide was not statistically significant at week 52. The initial fall in FPG with glyburide was greater than with AVANDIA; however, this effect was less durable over time.
The improvement in glycemic control seen with AVANDIA 4 mg twice daily at week 26 was maintained through week 52 of the study.
Figure 4. Mean FPG Over Time in a 52-Week Glyburide-Controlled Study
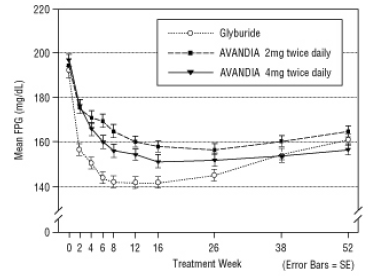
Figure 5. Mean HbA1c Over Time in a 52-Week Glyburide-Controlled Study
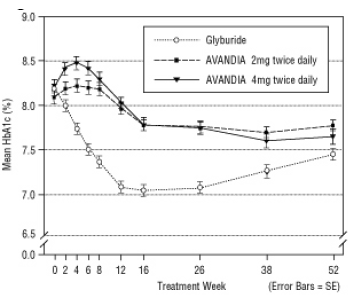
Hypoglycemia was reported in 12.1% of glyburide-treated patients versus 0.5% (2 mg twice daily) and 1.6% (4 mg twice daily) of patients treated with AVANDIA. The improvements in glycemic control were associated with a mean weight gain of 1.75 kg and 2.95 kg for patients treated with 2 mg and 4 mg twice daily of AVANDIA, respectively, versus 1.9 kg in glyburide-treated patients. In patients treated with AVANDIA, C-peptide, insulin, pro-insulin, and pro-insulin split products were significantly reduced in a dose-ordered fashion, compared to an increase in the glyburide-treated patients.
A Diabetes Outcome Progression Trial (ADOPT) was a multicenter, double-blind, controlled trial (N = 4,351) conducted over 4 to 6 years to compare the safety and efficacy of AVANDIA, metformin, and glyburide monotherapy in patients recently diagnosed with type 2 diabetes mellitus ( ≤ 3 years) inadequately controlled with diet and exercise. The mean age of patients in this trial was 57 years and the majority of patients (83%) had no known history of cardiovascular disease. The mean baseline FPG and HbA1c were 152 mg/dL and 7.4%, respectively. Patients were randomized to receive either AVANDIA 4 mg once daily, glyburide 2.5 mg once daily, or metformin 500 mg once daily, and doses were titrated to optimal glycemic control up to a maximum of 4 mg twice daily for AVANDIA, 7.5 mg twice daily for glyburide, and 1,000 mg twice daily for metformin. The primary efficacy outcome was time to consecutive FPG > 180 mg/dL after at least 6 weeks of treatment at the maximum tolerated dose of study medication or time to inadequate glycemic control, as determined by an independent adjudication committee.
The cumulative incidence of the primary efficacy outcome at 5 years was 15% with AVANDIA, 21% with metformin, and 34% with glyburide (hazard ratio 0.68 [95% CI 0.55, 0.85] versus metformin, HR 0.37 [95% CI 0.30, 0.45] versus glyburide).
Cardiovascular and adverse event data (including effects on body weight and bone fracture) from ADOPT for AVANDIA, metformin, and glyburide are described in WARNINGS AND PRECAUTIONS and ADVERSE REACTIONS, respectively. As with all medications, efficacy results must be considered together with safety information to assess the potential benefit and risk for an individual patient.
Combination With Metformin or Sulfonylurea
The addition of AVANDIA to either metformin or sulfonylurea resulted in significant reductions in hyperglycemia compared to either of these agents alone. These results are consistent with an additive effect on glycemic control when AVANDIA is used as combination therapy.
Combination With Metformin
A total of 670 patients with type 2 diabetes participated in two 26-week, randomized, double-blind, placebo/active-controlled studies designed to assess the efficacy of AVANDIA in combination with metformin. AVANDIA, administered in either once daily or twice daily dosing regimens, was added to the therapy of patients who were inadequately controlled on a maximum dose (2.5 grams/day) of metformin.
In one study, patients inadequately controlled on 2.5 grams/day of metformin (mean baseline FPG 216 mg/dL and mean baseline HbA1c 8.8%) were randomized to receive 4 mg of AVANDIA once daily, 8 mg of AVANDIA once daily, or placebo in addition to metformin. A statistically significant improvement in FPG and HbA1c was observed in patients treated with the combinations of metformin and 4 mg of AVANDIA once daily and 8 mg of AVANDIA once daily, versus patients continued on metformin alone (Table 10).
Table 10. Glycemic Parameters in a 26-Week Combination Study of AVANDIA Plus Metformin
| Metformin N = 113 | AVANDIA 4 mg once daily + metformin N = 116 | AVANDIA 8 mg once daily + metformin N = 110 | |
| FPG (mg/dL) | |||
| Baseline (mean) | 214 | 215 | 220 |
| Change from baseline (mean) | 6 | -33 | -48 |
| Difference from metformin alone (adjusted mean) | - | -40* | -53* |
| % of patients with ≥ 30 mg/dL decrease from baseline | 20% | 45% | 61% |
| HbA1c (%) | |||
| Baseline (mean) | 8.6 | 8.9 | 8.9 |
| Change from baseline (mean) | 0.5 | -0.6 | -0.8 |
| Difference from metformin alone (adjusted mean) | - | -1.0* | -1.2* |
| % of patients with ≥ 0.7% decrease from baseline | 11% | 45% | 52% |
| * p < 0.0001 compared to metformin. | |||
In a second 26-week study, patients with type 2 diabetes inadequately controlled on 2.5 grams/day of metformin who were randomized to receive the combination of AVANDIA 4 mg twice daily and metformin (N = 105) showed a statistically significant improvement in glycemic control with a mean treatment effect for FPG of -56 mg/dL and a mean treatment effect for HbA1c of -0.8% over metformin alone. The combination of metformin and AVANDIA resulted in lower levels of FPG and HbA1c than either agent alone.
Patients who were inadequately controlled on a maximum dose (2.5 grams/day) of metformin and who were switched to monotherapy with AVANDIA demonstrated loss of glycemic control, as evidenced by increases in FPG and HbA1c. In this group, increases in LDL and VLDL were also seen.
Combination With a Sulfonylurea
A total of 3,457 patients with type 2 diabetes participated in ten 24- to 26-week randomized, double-blind, placebo/active-controlled studies and one 2-year double-blind, active-controlled study in elderly patients designed to assess the efficacy and safety of AVANDIA in combination with a sulfonylurea. AVANDIA 2 mg, 4 mg, or 8 mg daily was administered, either once daily (3 studies) or in divided doses twice daily (7 studies), to patients inadequately controlled on a submaximal or maximal dose of sulfonylurea.
In these studies, the combination of AVANDIA 4 mg or 8 mg daily (administered as single or twice daily divided doses) and a sulfonylurea significantly reduced FPG and HbA1c compared to placebo plus sulfonylurea or further up-titration of the sulfonylurea. Table 11 shows pooled data for 8 studies in which AVANDIA added to sulfonylurea was compared to placebo plus sulfonylurea.
Table 11. Glycemic Parameters in 24- to 26-Week Combination Studies of AVANDIA Plus Sulfonylurea
| Twice Daily Divided Dosing (5 Studies) | Sulfonylurea N = 397 | AVANDIA 2 mg twice daily + sulfonylurea N = 497 | Sulfonylurea N = 248 | AVANDIA 4 mg twice daily + sulfonylurea N = 346 |
| FPG (mg/dL) | ||||
| Baseline (mean) | 204 | 198 | 188 | 187 |
| Change from baseline (mean) | 11 | -29 | 8 | -43 |
| Difference from sulfonylurea alone (adjusted mean) | - | -42* | - | -53* |
| % of patients with ≥ 30 mg/dL decrease from baseline | 17% | 49% | 15% | 61% |
| HbA1c (%) | ||||
| Baseline (mean) | 9.4 | 9.5 | 9.3 | 9.6 |
| Change from baseline (mean) | 0.2 | -1.0 | 0.0 | -1.6 |
| Difference from sulfonylurea alone (adjusted mean) | - | -1.1* | - | -1.4* |
| % of patients with ≥ 0.7% decrease from baseline | 21% | 60% | 23% | 75% |
| Once Daily Dosing(3 Studies) | Sulfonylurea N = 172 | AVANDIA 4 mg once daily + sulfonylurea N = 172 | Sulfonylurea N = 173 | AVANDIA 8 mg once daily + sulfonylurea N = 176 |
| FPG (mg/dL) | ||||
| Baseline (mean) | 198 | 206 | 188 | 192 |
| Change from baseline (mean) | 17 | -25 | 17 | -43 |
| Difference from sulfonylurea alone (adjusted mean) | - | -47* | - | -66* |
| % of patients with ≥ 30 mg/dL decrease from baseline | 17% | 48% | 19% | 55% |
| HbA1c (%) | ||||
| Baseline (mean) | 8.6 | 8.8 | 8.9 | 8.9 |
| Change from baseline (mean) | 0.4 | -0.5 | 0.1 | -1.2 |
| Difference from sulfonylurea alone (adjusted mean) | - | -0.9* | - | -1.4* |
| % of patients with ≥ 0.7% decrease from baseline | 11% | 36% | 20% | 68% |
| * p < 0.0001 compared to sulfonylurea alone. | ||||
One of the 24- to 26-week studies included patients who were inadequately controlled on maximal doses of glyburide and switched to 4 mg of AVANDIA daily as monotherapy; in this group, loss of glycemic control was demonstrated, as evidenced by increases in FPG and HbA1c.
In a 2-year double-blind study, elderly patients (aged 59 to 89 years) on half-maximal sulfonylurea (glipizide 10 mg twice daily) were randomized to the addition of AVANDIA (n = 115, 4 mg once daily to 8 mg as needed) or to continued up-titration of glipizide (n = 110), to a maximum of 20 mg twice daily. Mean baseline FPG and HbA1c were 157 mg/dL and 7.72%, respectively, for the AVANDIA plus glipizide arm and 159 mg/dL and 7.65%, respectively, for the glipizide up-titration arm. Loss of glycemic control (FPG ≥ 180 mg/dL) occurred in a significantly lower proportion of patients (2%) on AVANDIA plus glipizide compared to patients in the glipizide up-titration arm (28.7%). About 78% of the patients on combination therapy completed the 2 years of therapy while only 51% completed on glipizide monotherapy. The effect of combination therapy on FPG and HbA1c was durable over the 2-year study period, with patients achieving a mean of 132 mg/dL for FPG and a mean of 6.98% for HbA1c compared to no change on the glipizide arm.
Combination With Sulfonylurea Plus Metformin
In two 24- to 26-week, double-blind, placebo-controlled, studies designed to assess the efficacy and safety of AVANDIA in combination with sulfonylurea plus metformin, AVANDIA 4 mg or 8 mg daily, was administered in divided doses twice daily, to patients inadequately controlled on submaximal (10 mg) and maximal (20 mg) doses of glyburide and maximal dose of metformin (2 g/day). A statistically significant improvement in FPG and HbA1c was observed in patients treated with the combinations of sulfonylurea plus metformin and 4 mg of AVANDIA and 8 mg of AVANDIA versus patients continued on sulfonylurea plus metformin, as shown in Table 12.
Table 12. Glycemic Parameters in a 26-Week Combination Study of AVANDIA Plus Sulfonylurea and Metformin
| Sulfonylurea + metformin N = 273 | AVANDIA 2 mg twice daily + sulfonylurea + metformin N = 276 | AVANDIA 4 mg twice daily + sulfonylurea + metformin N = 277 | |
| FPG (mg/dL) | |||
| Baseline (mean) | 189 | 190 | 192 |
| Change from baseline (mean) | 14 | -19 | -40 |
| Difference from sulfonylurea plus metformin (adjusted mean) | - | -30* | -52* |
| % of patients with ≥ 30 mg/dL decrease from baseline | 16% | 46% | 62% |
| HbA1c (%) | |||
| Baseline (mean) | 8.7 | 8.6 | 8.7 |
| Change from baseline (mean) | 0.2 | -0.4 | -0.9 |
| Difference from sulfonylurea plus metformin (adjusted mean) | - | -0.6* | -1.1* |
| % of patients with ≥ 0.7% decrease from baseline | 16% | 39% | 63% |
| * p < 0.0001 compared to placebo. | |||
References
- Food and Drug Administration Briefing Document. Joint meeting of the Endocrino Metabolic Drugs and Drug Safety and Risk Management Advisory Committees. Ju 2007.
- DREAM Trial Investigators. Effect of rosiglitazone on the frequency of diabetes in with impaired glucose tolerance or impaired fasting glucose: a randomised controll Lancet 2006;368:1096-1105.
- Home PD, Pocock SJ, Beck-Nielsen H, et al. Rosiglitazone evaluated for cardiovas outcomes - an interim analysis. NEJM 2007;357:1-11.
- Park JY, Kim KA, Kang MH, et al. Effect of rifampin on the pharmacokinetics of rosiglitazone in healthy subjects. Clin Pharmacol Ther 2004;75:157-162.
How Supplied/Storage and Handling
Each pentagonal film-coated TILTAB tablet contains rosiglitazone as the maleate as follows: 2 mg-pink, debossed with SB on one side and 2 on the other; 4 mg-orange, debossed with SB on one side and 4 on the other; 8 mg-red-brown, debossed with SB on one side and 8 on the other.
- 2 mg bottles of 60: NDC 0029-3158-18
- 4 mg bottles of 30: NDC 0029-3159-13
- 4 mg bottles of 90: NDC 0029-3159-00
- 8 mg bottles of 30: NDC 0029-3160-13
- 8 mg bottles of 90: NDC 0029-3160-59
Store at 25 C (77°F); excursions 15 to 30 C (59 to 86 F). Dispense in a tight, light-resistant container.
last updated 02/2008
Avandia, rosiglitazone maleate, patient information (in plain English)
Detailed Info on Signs, Symptoms, Causes, Treatments of Diabetes
The information in this monograph is not intended to cover all possible uses, directions, precautions, drug interactions or adverse effects. This information is generalized and is not intended as specific medical advice. If you have questions about the medicines you are taking or would like more information, check with your doctor, pharmacist, or nurse.
back to: Browse all Medications for Diabetes
APA Reference
Staff, H.
(2008, February 28). Avandia for Treatment of Diabetes - Avandia Full Prescribing Information, HealthyPlace. Retrieved
on 2026, April 2 from https://www.healthyplace.com/diabetes/medications/avandia-diabetes-treatment-information